The False Claims Act: How It Works and Why ABA Is Now a Target
WASHINGTON, D.C. — the federal False Claims Act, originally enacted during the Civil War to combat defense contractor fraud, has become the single most powerful enforcement tool in American healthcare. The law imposes liability on individuals and companies that knowingly submit false claims for payment to government programs, including Medicaid and Medicare. Its qui tam provisions allow private citizens with knowledge of fraud — called relators — to file lawsuits on behalf of the United States government and receive between 15 and 30 percent of whatever the government successfully recovers.
In fiscal year 2024, the Department of Justice recovered $2.9 billion through FCA enforcement — the highest total in a decade and the sixteenth consecutive year of recoveries exceeding $2 billion. Healthcare accounted for over $1.67 billion, or 57 percent, of total FCA recoveries. Whistleblowers filed a record 979 qui tam cases, the highest number since the DOJ began keeping records in 1987. Relators received over $400 million in awards, with more than $261 million going to whistleblowers in healthcare matters specifically.
The overall number of new FCA matters opened in fiscal year 2024 reached an all-time high of 1,402, topping the previous record from fiscal year 2023 by 15 percent. The DOJ opened 423 matters on its own initiative — the second-highest on record — while qui tam lawsuits accounted for the remaining 979. Resolutions of qui tam cases yielded over $2.4 billion, representing 82 percent of total FCA recoveries.
Whistleblowers filed 979 qui tam cases in FY 2024 — the highest ever. Healthcare accounted for $1.67 billion of $2.9 billion in total FCA recoveries. The legal infrastructure for ABA-specific whistleblower lawsuits is already built.
How FCA Liability Triggers in ABA
The Keller Grover law firm published a detailed analysis in January 2026 identifying the specific types of FCA violations that occur in ABA therapy. The firm’s analysis maps directly to the findings in the HHS-OIG state audits and provides a roadmap for whistleblowers considering qui tam actions against ABA providers.
Inadequate supervision: ABA regulations require that Board Certified Behavior Analysts or other qualified professionals directly supervise paraprofessional therapy technicians at specified ratios and frequencies. Billing for properly supervised services while actually providing inadequate supervision constitutes fraud. Whistleblowers may observe behavior analysts supervising far more technicians than regulations allow, billing for supervision that does not occur, or providing only cursory supervision that does not meet clinical or regulatory standards.
Services without medical necessity: providers must establish medical necessity before delivering therapy services. Employees may witness providers continuing intensive therapy without clinical justification, or billing for standardized hour blocks regardless of the child’s actual needs or progress.
Fabricated documentation: some providers create false clinical documentation to support claims for services that did not occur, were not medically necessary, or did not meet regulatory requirements. The Massachusetts indictment of Lamour by Design in June 2025 is a direct example of this category.
Billing for unqualified staff: submitting claims for services delivered by individuals who lack required credentials — such as behavioral technicians without the mandated 40-hour training or competency assessment — can constitute a false claim under the FCA. The Colorado OIG audit estimated that 1,500 to 2,000 technicians in the state may be working without required certification.
The Whistleblower Law Collaborative: ABA as an Emerging Enforcement Category

Law firms specializing in qui tam litigation are actively publishing guides on ABA-specific False Claims Act violations, signaling a new wave of enforcement activity.
The Whistleblower Law Collaborative published an analysis in 2025, co-authored by attorney Erica Blachman Hitchings and originally appearing in Law360, that characterized the Colorado OIG audit as a roadmap for the most common and actionable types of Medicaid fraud in the ABA industry. The analysis highlighted improper staffing, documentation failures, billing for nontherapy activities, and ineffective state oversight as categories of conduct that could support FCA claims.
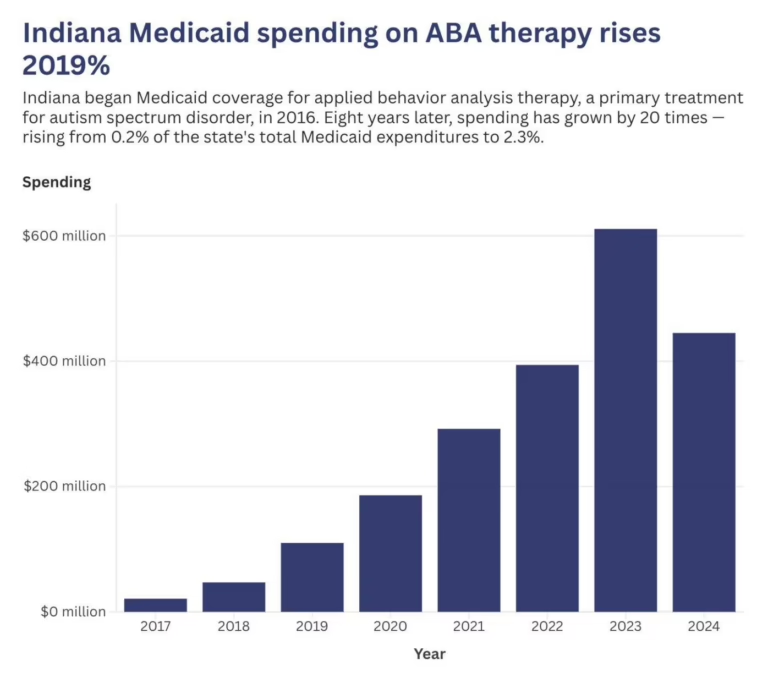
The Collaborative’s analysis noted that autism diagnoses among 8-year-olds have climbed to 1 in 31, and that as diagnoses increase, so has Medicaid spending. Colorado’s ABA Medicaid spending jumped from $60.1 million in 2019 to $163.5 million by 2023 — a trend mirrored nationally. The combination of rapid spending growth, documented billing irregularities, and insufficient state oversight creates the conditions that FCA litigation is designed to address.
For potential whistleblowers working inside ABA providers, the qui tam process involves specific procedures. Complaints are filed under seal, keeping them confidential while the DOJ investigates. This seal period typically lasts months or years as government attorneys examine evidence and decide whether to intervene. If the government intervenes, it takes over prosecution; if it declines, the relator may proceed independently. Relators receive between 15 and 30 percent of government recoveries depending on whether the government intervenes.
Behavioral Health FCA Settlements: The Precedents
FCA settlements in behavioral health are already occurring. In fiscal year 2024, six health facilities providing behavioral health services paid $16.6 million to resolve allegations that they knowingly billed for inpatient behavioral health services that were medically unnecessary or that otherwise did not comply with federal and state regulations. In a separate case, a behavioral health services provider in Georgia settled for $750,000 after a whistleblower filed a qui tam complaint alleging fabricated documentation, inflated service hours, and billing for services never rendered. The relator received a 23 percent share.
In Massachusetts, a $25 million settlement was reached with a private equity firm and former mental health center executives over allegations of unlicensed and unsupervised patient care. Kevin Lownds of the Massachusetts MFCU handled the case. The settlement — described as the largest of its kind — was triggered by a whistleblower complaint from a former employee.
These precedents establish that behavioral health providers, including those backed by private equity, face real financial exposure under the FCA. The combination of documented audit findings, active MFCU enforcement, and law firm recruitment of insider whistleblowers creates a compounding enforcement risk that will intensify as the OIG’s remaining state audits are completed.
The Constitutional Challenge: Zafirov and the Future of Qui Tam
One significant legal development could affect the trajectory of FCA whistleblower lawsuits. In September 2024, a federal district court in Florida held in United States ex rel. Zafirov v. Florida Medical Associates that the qui tam provisions of the FCA violate the Appointments Clause of the Constitution by creating self-appointed officers of the United States. The case is on appeal before the Eleventh Circuit and could ultimately reach the Supreme Court.
If the qui tam provision is invalidated, the FCA would still exist as an enforcement tool, but the government itself would need to initiate all cases. The whistleblower bar has expressed concern that this would dramatically reduce enforcement capacity, while the defense bar argues that relators currently have too much power. For ABA providers, the outcome of Zafirov will determine whether the anticipated wave of whistleblower lawsuits materializes in its expected form, or whether enforcement shifts to a government-initiated model.
What ABA Providers Should Do Now
For ABA providers, the FCA risk environment requires immediate operational attention. Providers should conduct internal compliance audits focused on the specific deficiency categories identified in the OIG state audits: session note quality, supervision documentation, credentialing verification, medical necessity documentation, and time-tracking accuracy. Providers should ensure that their compliance programs include mechanisms for employees to report concerns internally before turning to external channels.
Providers backed by private equity face elevated risk. Massachusetts has specifically amended its FCA to focus on PE and corporate ownership in healthcare, and federal enforcement officials have identified PE investments in healthcare as a priority area. The combination of the audit trail created by the OIG series, the recruitment efforts of whistleblower law firms, and the public statements of enforcement officials like Kevin Lownds creates a convergence of risk factors that should be addressed proactively rather than reactively.
AT A GLANCE
| FCA FY 2024 recoveries: | $2.9 billion total; $1.67 billion from healthcare (DOJ) |
|---|---|
| Qui tam cases filed: | 979 in FY 2024 — all-time record since 1987 |
| Whistleblower awards: | $400M+ total; $261M+ in healthcare matters |
| Relator share: | 15–30% of government recoveries under qui tam provisions |
| Key ABA FCA triggers: | Inadequate supervision, fabricated documentation, unqualified staff, billing for nontherapy time |
| Behavioral health settlements: | $16.6M (6 facilities, FY 2024); $750K (Georgia qui tam); $25M (MA PE-backed provider) |
| MA enforcement: | Kevin Lownds, MFCU Division Chief, called ABA fraud “rampant” (AHLA Forum, October 2025) |
| Constitutional challenge: | Zafirov v. Florida Medical Associates — qui tam provision challenged; pending Eleventh Circuit appeal |
| Law firm activity: | Keller Grover, Whistleblower Law Collaborative publishing ABA-specific FCA guides (2025–2026) |
| New FCA matters: | 1,402 total in FY 2024 — all-time high |
SOURCES & REFERENCES
| 1. | DOJ. False Claims Act statistics. FY 2024. Reported by Akerman LLP, “HRx: False Claims Act Enforcement Trends in Healthcare: FY 2024.” February 4, 2025. akerman.com |
|---|---|
| 2. | Keller Grover. “False Claims Act Violations in ABA Therapy Treatment for Autism.” January 28, 2026. kellergrover.com |
| 3. | Whistleblower Law Collaborative. “Medicaid Fraud Risks in ABA Therapy.” Law360 / WLC. 2025. whistleblowerllc.com |
| 4. | Massachusetts AG’s Office. “AG’s Office Secures Indictments Against Randolph Autism Service Provider.” June 10, 2025. mass.gov |
| 5. | Morgan Lewis. “Applied Behavioral Analysis: Key Service for Children with Autism Is Under Payment Scrutiny.” November 14, 2025. morganlewis.com |
| 6. | DOJ / Southern District of Texas. “Mental health services providers pay over a million to settle false claims liability.” July 2024. justice.gov |
| 7. | Bracker & Marcus. “Behavioral Health Services Provider Settles False Claims Act Allegations for $750,000.” October 31, 2025. fcacounsel.com |
| 8. | Massachusetts AG’s Office. “Private Equity Firm and Former Mental Health Center Executives Pay $25 Million.” October 2021. mass.gov |
| 9. | American Conference Institute. “False Claims and Qui Tam Enforcement — FY 2024 Overview.” americanconference.com |