The Indictment: Lamour by Design and Lamour Community Health Institute
RANDOLPH, MASSACHUSETTS — on June 10, 2025, the Massachusetts Attorney General’s Office announced that the Statewide Grand Jury had returned indictments against Patrice Lamour and her two Randolph-based companies, Lamour by Design and Lamour Community Health Institute, for fraudulently billing MassHealth more than $1 million for services that were never provided. Each defendant was indicted on one count of Medicaid False Claims and one count of Larceny over $1,200.
Lamour by Design primarily received payment from MassHealth for applied behavioral analysis services, a treatment principally designed for children with autism spectrum disorder. According to the Attorney General’s Office, the defendants fabricated documentation to support false claims for ABA services that were never actually delivered to patients. The indictment represents one of the first criminal prosecutions in Massachusetts specifically targeting an ABA provider for Medicaid fraud.
The case was handled by the Massachusetts Medicaid Fraud Division, which receives 75 percent of its funding from the U.S. Department of Health and Human Services under a grant totaling $5.9 million for federal fiscal year 2025, with the remaining 25 percent funded by the Commonwealth. The Medicaid Fraud Control Unit is a specialized enforcement arm certified annually by HHS to investigate and prosecute healthcare providers who defraud the state Medicaid program.
The distinction between the Lamour indictment and the HHS-OIG state audits is categorical: the audits identify documentation deficiencies and improper payments, while the Massachusetts case alleges intentional fabrication of records to support claims for services that never occurred.
Kevin Lownds and the MFCU: ABA Fraud Is Rampant
The Lamour indictment did not emerge in isolation. Kevin Lownds, Division Chief at the Medicaid Fraud Division of the Massachusetts Attorney General’s Office, has publicly identified ABA therapy as an enforcement priority. At the American Health Lawyer’s Association Fraud and Compliance Forum in October 2025, Lownds stated that ABA therapy is an area of behavioral health where fraud and abuse is rampant.
Lownds noted specifically that the high reimbursement rates associated with ABA services have enticed potential fraudsters into the space. He went further, stating that his unit was often seeing fraud warranting criminal charges, most often in cases where providers were billing for services that were never actually provided to patients. This characterization is significant because it draws a distinction between documentation deficiencies — the primary finding in the HHS-OIG state audits — and outright fabrication of service records.
At the May 2025 Boston Bar Association White Collar Crime Conference, Lownds described a good working relationship between the state MFCU and federal prosecutors, noting that the office collaborates with the U.S. Attorney’s Office when appropriate and makes independent enforcement decisions when appropriate. He cited recent enforcement trends related to private equity investments in healthcare and observed that Massachusetts had recently amended its False Claims Act to specifically focus on private equity and corporate ownership in healthcare.
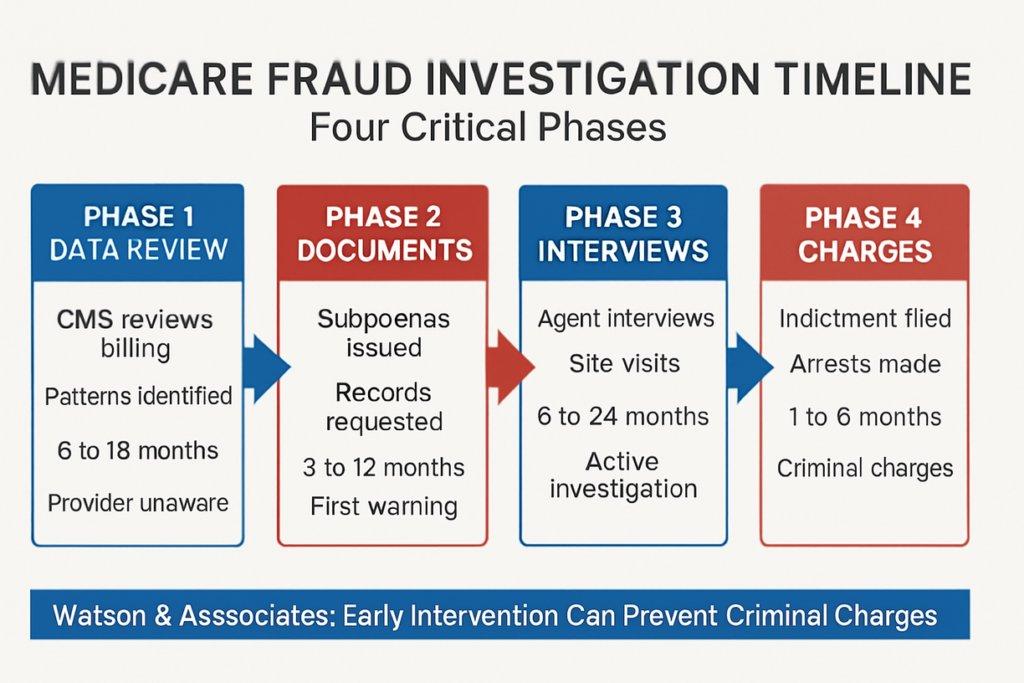
State Medicaid Fraud Control Units have publicly identified ABA therapy as an enforcement priority, with Massachusetts leading criminal prosecution efforts.
The Legal Framework: Medicaid False Claims vs. Documentation Deficiencies
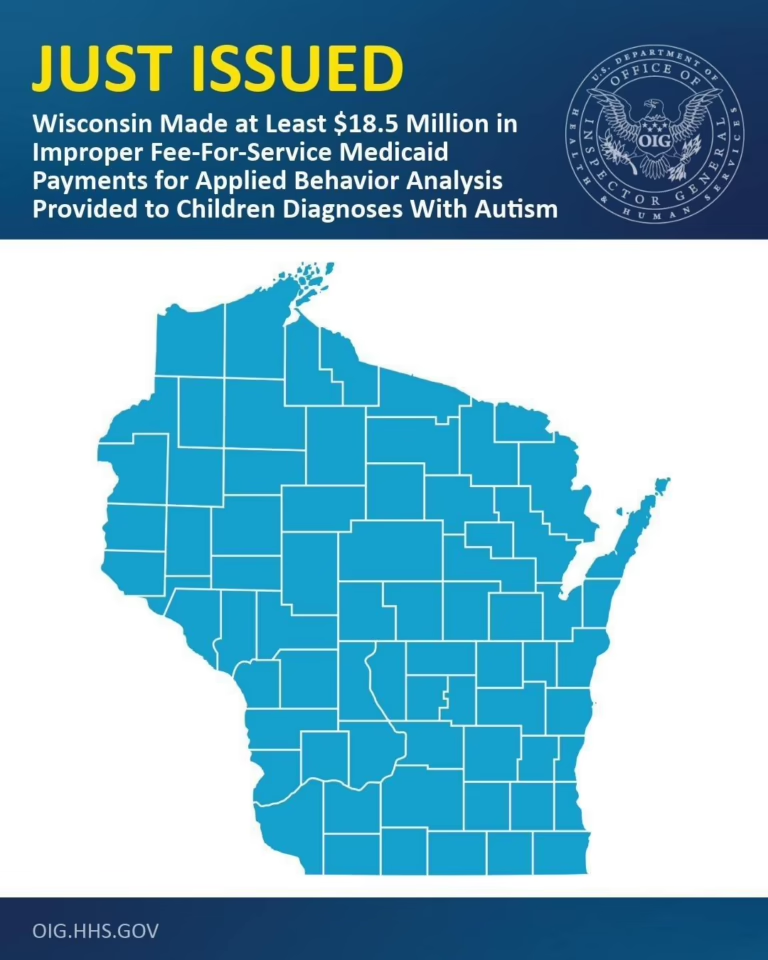
The legal distinction between billing errors, documentation deficiencies, and outright fraud is critical for ABA providers to understand. The HHS-OIG state audits have primarily identified documentation failures: session notes that do not adequately describe services, missing signatures, billing for nontherapy time, and services delivered by providers without appropriate credentials. These findings trigger repayment obligations but are generally treated as compliance failures rather than criminal conduct.
Criminal fraud charges require a higher evidentiary threshold. Prosecutors must demonstrate that the provider knowingly submitted false claims for services that were not provided, or that the provider intentionally fabricated documentation to support claims that would not otherwise be payable. The Lamour indictment alleges both: fabrication of documentation and submission of false claims for services never rendered.
For ABA providers, the escalation from audit findings to criminal prosecution represents a qualitative shift in enforcement posture. The Morgan Lewis law firm, in a November 2025 analysis, noted that the increased enforcement scrutiny arriving in the ABA space is not surprising given the increased audit activity by HHS-OIG, and that providers should plan accordingly for MFCU investigations in states where Medicaid programs cover ABA with high reimbursement rates.
The Broader Enforcement Landscape
Massachusetts is not the only state with active ABA enforcement. The broader Medicaid fraud enforcement landscape shows increasing attention to behavioral health billing practices. At the AHLA Forum, Assistant Attorney General Raja Mishra from Maryland’s MFCU joined Lownds in highlighting behavioral health and medical transportation as areas rife with fraud and abuse.
The combination of HHS-OIG audit findings, state MFCU criminal investigations, and growing congressional interest in Medicaid program integrity creates a multi-layered enforcement environment for ABA providers. Providers face potential exposure to federal audit repayment demands, state criminal prosecution, civil False Claims Act liability, and administrative actions including exclusion from Medicaid participation.
For the broader ABA industry, the Massachusetts indictment sends a clear message: the enforcement posture has shifted from compliance guidance to criminal prosecution. Providers whose documentation practices would not survive a Lownds-level investigation should treat this as an urgent operational priority.
AT A GLANCE
| Defendant: | Patrice Lamour; Lamour by Design (LBD); Lamour Community Health Institute (LCHI) |
|---|---|
| Location: | Randolph, Massachusetts |
| Indictment date: | June 10, 2025 |
| Charges: | 1 count Medicaid False Claims + 1 count Larceny over $1,200 (each defendant) |
| Alleged amount: | More than $1 million in false MassHealth claims |
| Alleged conduct: | Fabricated documentation; billed for ABA services never provided |
| Key enforcement figure: | Kevin Lownds, Division Chief, MA MFCU |
| Lownds on ABA fraud: | Called ABA fraud “rampant” at AHLA Forum (October 2025) |
| MA FCA amendment: | Massachusetts amended its False Claims Act to focus on PE/corporate ownership in healthcare |
| MFCU funding: | $5.9M federal + $1.97M state for FY 2025 |
SOURCES & REFERENCES
| 1. | Massachusetts AG’s Office. “AG’s Office Secures Indictments Against Randolph Autism Service Provider for Allegedly Submitting More Than $1 Million in False Claims.” June 10, 2025. mass.gov |
|---|---|
| 2. | Morgan Lewis. “Applied Behavioral Analysis: Key Service for Children with Autism Is Under Payment Scrutiny.” November 14, 2025. morganlewis.com/blogs/healthlawscan |
| 3. | Morgan Lewis. “Enforcement Notes from American Health Law Association’s Fraud and Compliance Forum.” October 16, 2025. morganlewis.com/blogs/healthlawscan |
| 4. | Morgan Lewis. “Mass. USAO Focuses on Healthcare Fraud in Private Equity Investments, Broker Arrangements at Annual Conference.” May 19, 2025. morganlewis.com/blogs/healthlawscan |
| 5. | HHS-OIG. “Audits of Medicaid Applied Behavior Analysis for Children Diagnosed With Autism.” Series SRS-A-25-029. oig.hhs.gov |