ABA Enters the Federal Fraud Spotlight
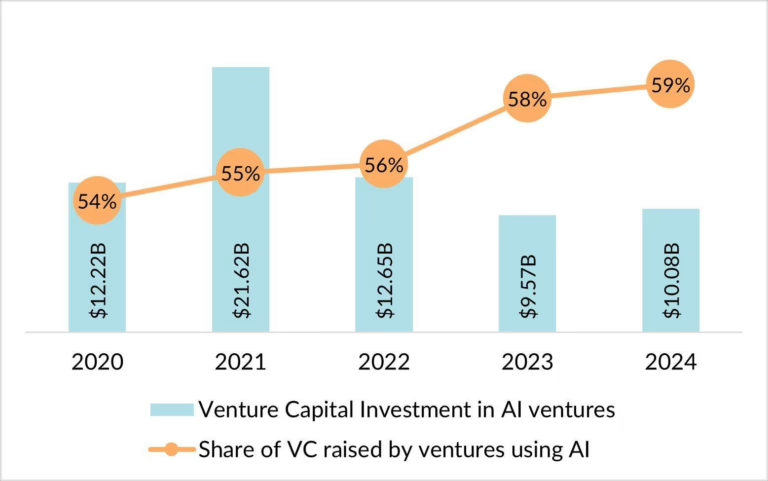
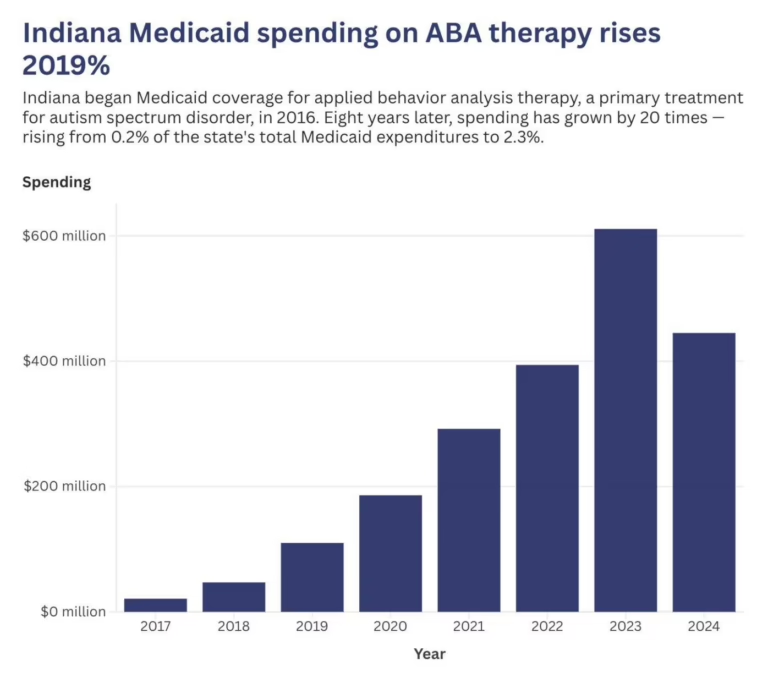
WASHINGTON, D.C. — The ABA therapy industry has operated for most of its history in a regulatory environment defined primarily by state-level oversight, BACB credentialing standards, and payer-specific authorization requirements. Federal involvement was limited to Medicaid program administration and occasional OIG audits. That era is over. CMS Administrator Dr. Mehmet Oz has made healthcare fraud a centerpiece of his tenure, and ABA therapy — with its four-state audit trail of 100 percent error rates, $600 million-plus in improper payments, and explosive spending growth from $660 million to $2.2 billion in Medicaid expenditures between 2019 and 2023 — has attracted the kind of federal attention that changes industries.
The Whistleblower Law Collaborative, in its analysis of the Colorado OIG audit, cited Oz as identifying ABA fraud as a massive problem. The characterization is significant because it positions ABA billing irregularities alongside the hospice fraud, DME fraud, and home health fraud schemes that Oz has been publicly investigating through field visits, press conferences, and social media campaigns in California, Florida, Minnesota, Maine, and New York.
On February 25, 2026, the Trump Administration announced what it described as a major crackdown on healthcare fraud, led by Oz and HHS Secretary Robert F. Kennedy Jr. The announcement included three components with direct implications for ABA providers: first, deferring $259.5 million in quarterly federal Medicaid funding in Minnesota to prevent payment of questionable claims; second, a six-month moratorium on new Medicare enrollment for DMEPOS suppliers; and third, the launch of CRUSH — Comprehensive Regulations to Uncover Suspicious Healthcare — a request for information seeking input on preventing, detecting, and responding to fraud across Medicare, Medicaid, CHIP, and the health insurance marketplace.
CMS announced that approximately $300 billion per year is lost to fraud, waste, and abuse across federal health programs, and the agency launched what it described as the largest anti-fraud initiative in its history. The initiative includes data-driven detection, stepped-up claims audits, tighter provider enrollment rules, and closer coordination with law enforcement and state Medicaid agencies. While ABA represents a fraction of total Medicaid spending, the sector’s growth rate, error rate, and media visibility make it a high-profile target.
CMS Administrator Mehmet Oz identified ABA therapy fraud as a massive problem. The characterization positions ABA billing irregularities alongside the hospice, DME, and home health fraud schemes that Oz has been publicly investigating. — Whistleblower Law Collaborative, March 2026
What Federal Attention Means for ABA Providers
The DOJ launched a new Division for National Fraud Enforcement in January 2026, creating dedicated prosecutorial capacity for healthcare fraud cases. The Whistleblower Law Collaborative noted that given the OIG’s ongoing multi-state review of ABA programs and the explosive growth of the industry, whistleblowers with inside knowledge of ABA billing practices are more important than ever. Keller Grover, another firm specializing in False Claims Act litigation, published a detailed analysis of how ABA-specific FCA violations work, including billing for services by unqualified personnel, inadequate supervision, and documentation that does not support billed services.
The enforcement infrastructure being built around Medicaid fraud — CRUSH, the DOJ division, state-level Medicaid Fraud Control Units, OIG audit series — creates multiple vectors of accountability for ABA providers. A single billing irregularity can now trigger a federal OIG audit finding, a state-level recovery action, a DOJ criminal investigation, a whistleblower qui tam lawsuit, or some combination of all four. The regulatory environment has shifted from reactive oversight to proactive enforcement.
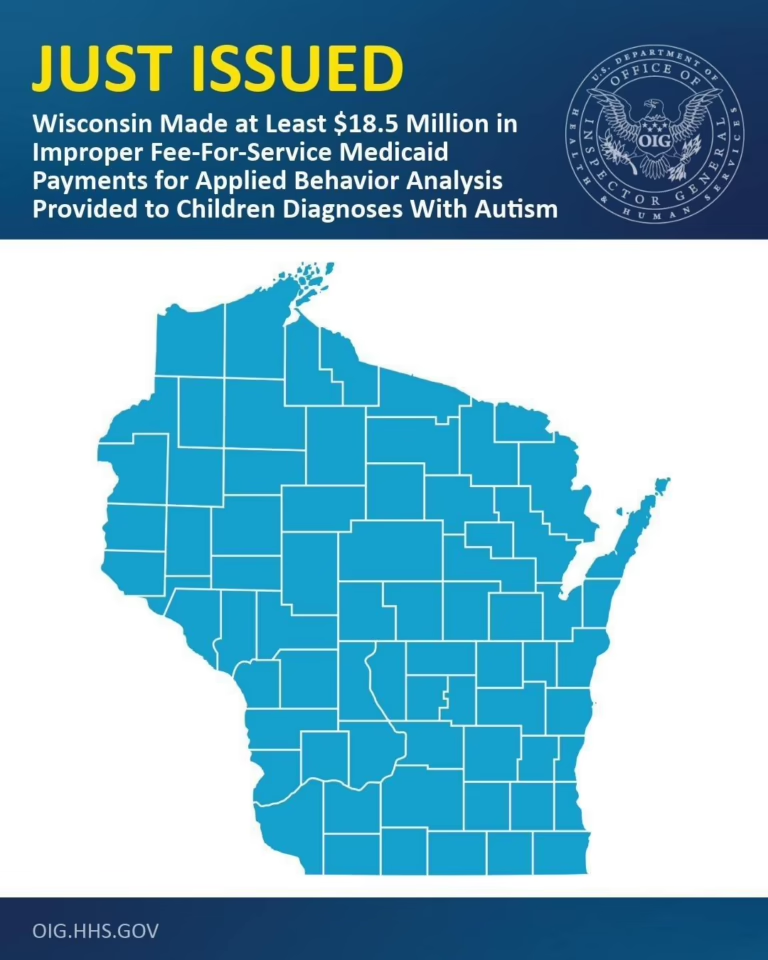
For ABA providers, the practical implications are immediate. Provider enrollment will face greater scrutiny, with the possibility of enrollment moratoriums in high-fraud states. Prior authorization requirements will tighten as states respond to OIG recommendations. Post-payment review — which Wisconsin never conducted in nearly a decade of ABA billing — will become standard. Documentation standards will be enforced rather than merely published. And whistleblower protections will encourage current and former employees to report billing irregularities directly to federal prosecutors.
Epstein Becker Green, analyzing Oz’s investigation of New York’s Medicaid program, warned that regardless of whether it is CMS, HHS, DOJ, or state Medicaid Fraud Control Units that come knocking, the government is fully prepared to combat fraud, waste, and abuse in healthcare. The firm emphasized that compliance programs continue to be essential for healthcare stakeholders and providers.
The political dynamics add another layer of complexity. Oz’s fraud campaign has been criticized by some Democratic governors as politically motivated, with Maine’s governor calling his letter a pretense for federal overreach. Minnesota filed a federal lawsuit against Oz, CMS, HHS, and Kennedy for withholding Medicaid funding. But the underlying audit findings are nonpartisan: the 100 percent error rates across four states were documented by career OIG auditors, not political appointees. The ABA industry cannot dismiss the enforcement environment as political theater when the audit trail is this comprehensive.

The Compliance Imperative
Benesch’s analysis concluded that the ABA sector is undergoing rapid regulatory recalibration, and that providers who invest now in compliance, transparency, and clinically sound service models will not only reduce legal and financial exposure but also reinforce trust across the Medicaid and private payer landscape. The firm recommended that providers reassess clinical practices, audit readiness, and financial structures to ensure long-term viability in this increasingly scrutinized environment.
The Whistleblower Law Collaborative’s analysis of the Colorado audit serves as a roadmap for the most common and actionable types of Medicaid fraud occurring in the ABA industry. It highlights how lax oversight creates fertile ground for False Claims Act cases. For compliance officers, the message is clear: the window for voluntary compliance improvement is closing. Providers that have not conducted internal audits, standardized their documentation, verified their staff credentials, and aligned their billing with their clinical records are operating in an environment where every level of government — from county prosecutors to the CMS Administrator — is looking for exactly those failures.
AT A GLANCE
| Oz quote: | ABA fraud is “a massive problem” (Whistleblower Law Collaborative) |
|---|---|
| CMS fraud estimate: | 00B/year lost to fraud, waste, abuse across federal health programs |
| CRUSH initiative: | RFI on preventing, detecting fraud in Medicare, Medicaid, CHIP; comments due March 30, 2026 |
| MN deferral: | 59.5M quarterly Medicaid funding deferred |
| DMEPOS moratorium: | 6-month freeze on new Medicare enrollment |
| DOJ division: | Division for National Fraud Enforcement launched January 2026 |
| ABA Medicaid spending: | 60M (2019) to .2B (2023); fastest-growing Medicaid service |
| OIG audit results: | 100% error rate across all 4 states audited; 00M+ improper payments |
| Whistleblower risk: | FCA qui tam cases; 15–30% awards; Keller Grover and Sanford Heisler active |
SOURCES & REFERENCES
| 1. | Whistleblower Law Collaborative. “Medicaid Fraud Risks in ABA Therapy.” March 2026. (Oz “massive problem” quote.) |
|---|---|
| 2. | Prism News. “Dr. Oz orders biggest CMS anti-fraud crackdown after 00B finding.” February 26, 2026. |
| 3. | Epstein Becker Green. “Dr. Mehmet Oz Announces Investigation Into NY Medicaid.” March 2026. |
| 4. | Fierce Healthcare. “Dr. Oz escalates Medicaid fraud claims against states.” March 2026. |
| 5. | Benesch. “Heightened Scrutiny of Medicaid-Funded ABA Services.” March 2026. |
| 6. | Keller Grover. “False Claims Act Violations in ABA Therapy Treatment for Autism.” January 28, 2026. |
| 7. | KFF Health News. “Oz escalates Medicaid fraud claims after focus on Minnesota.” March 2026. |