How Supervision Fraud Works
WASHINGTON, D.C. — ABA therapy regulations require that Board Certified Behavior Analysts or other qualified professionals directly supervise paraprofessional therapy technicians at specified ratios and frequencies. The BACB’s ethical standards require BCBAs to provide ongoing supervision, conduct regular observations of technician performance, review session data, and ensure that treatment protocols are being implemented with fidelity. Supervision is not optional; it is the clinical infrastructure that ensures ABA therapy is delivered safely and effectively.
Keller Grover’s January 2026 analysis of False Claims Act violations in ABA therapy identified supervision fraud as one of the most common and actionable categories of Medicaid billing fraud. The firm described the mechanics: billing for properly supervised services while actually providing inadequate supervision constitutes fraud. Whistleblowers may observe behavior analysts supervising far more technicians than regulations allow, billing for supervision that does not occur, or providing only cursory supervision that does not meet clinical or regulatory requirements.
The supervision fraud problem has two dimensions. The first is volume: BCBAs carrying caseloads that make meaningful supervision impossible. When a BCBA is assigned 15 or 20 or more technicians, the mathematical reality is that each technician receives only a fraction of the supervision time required by BACB standards and state regulations. The second dimension is documentation: supervision sessions that are billed to Medicaid but that consist of brief check-ins, clipboard reviews, or signature-only encounters rather than the direct observation, data review, and clinical decision-making that supervision requires.
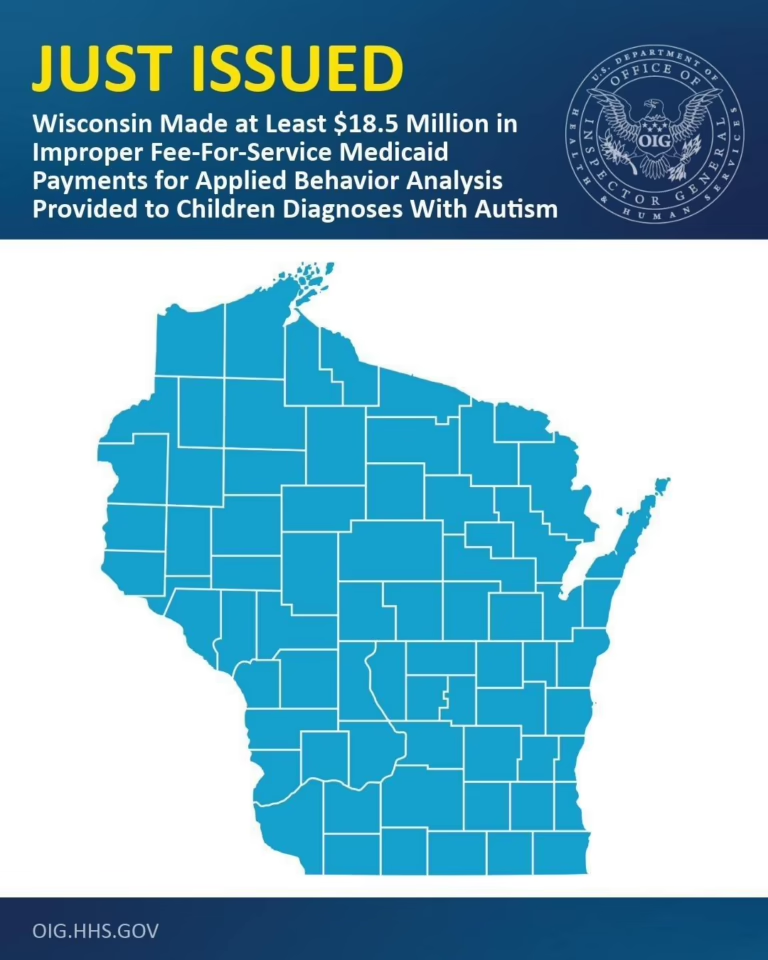
The OIG audits found these patterns across every state examined. The common error categories include services billed without evidence that required supervision was provided, supervision billed at the BCBA rate when the supervising clinician was not present during the session, and treatment modifications documented under CPT 97155 without evidence that a qualified supervisor actually evaluated the client and made clinical decisions. The Wisconsin audit specifically recommended that the state develop procedures to verify the provider who rendered the service and pay claims based on the rendering provider’s specialty level — a recommendation that implies the state was paying BCBA-level rates for services rendered by technicians without BCBA-level oversight.
Whistleblowers may observe behavior analysts supervising far more technicians than regulations allow, billing for supervision that doesn’t occur, or providing only cursory supervision that doesn’t meet the standard. — Keller Grover, False Claims Act analysis, January 2026
The Minnesota Criminal Case
The most extreme documented example of supervision fraud is a Minnesota criminal prosecution in which federal prosecutors charged a provider in a scheme that used unqualified behavioral technicians — often young adult relatives without autism-related training — to deliver purported one-on-one ABA therapy. The scheme involved inflating claims, forging supervisory signatures, and submitting bills for services not rendered, yielding more than $14 million from state Medicaid and a private health plan. The provider pled guilty in March 2026.
Sanford Heisler Sharp, a whistleblower firm, noted that the Minnesota charging document shows proceeds came not only from Medicaid but also from a private insurer, indicating that improper ABA practices can trigger parallel risk across public and private payers. The case demonstrates that supervision fraud is not merely a documentation issue; in its most egregious form, it involves deliberate falsification of credentials, forged signatures, and fictitious service records.
Minnesota had 85 open investigations into autism providers as of 2025, following FBI raids on two ABA providers in December 2024. The state launched a third-party audit of 14 types of Medicaid services deemed high-risk for fraud and delayed payments for those services for up to 90 days. The severity of Minnesota’s enforcement response reflects the severity of the fraud documented: this is not a state that found paperwork errors. This is a state that found criminal enterprises operating within the ABA Medicaid benefit.

Where Liability Falls
The liability chain in supervision fraud extends from the individual BCBA who signs off on sessions they did not observe, through the clinical director who assigns caseloads that make adequate supervision impossible, to the practice owner or PE sponsor that creates the financial incentives driving the behavior. Keller Grover noted that the False Claims Act imposes liability on individuals and companies that defraud government programs, and that whistleblowers may be awarded between 15 and 30 percent of what the government successfully recovers.
For BCBAs, signing supervision documentation for sessions they did not observe is both an ethical violation under the BACB Ethics Code and a potential criminal act if it results in false claims submitted to Medicaid. The BACB’s enforcement process can revoke certification, but the legal exposure extends far beyond professional discipline. BCBAs who participate in supervision fraud — even passively, by signing documentation under production pressure — face potential liability under the False Claims Act, state Medicaid fraud statutes, and in criminal cases, federal fraud charges.
For provider organizations, the liability is compounded. Companies that create caseload structures requiring BCBAs to supervise more technicians than they can meaningfully oversee are creating the conditions for supervision fraud. Companies that set productivity targets requiring BCBAs to bill for supervision they cannot deliver are incentivizing fraudulent documentation. Companies that do not audit supervision records or verify that supervision actually occurred are failing to implement the compliance controls that could detect and prevent the fraud.
For PE sponsors, the liability question is whether they knew or should have known that the operating models they were funding would produce supervision ratios incompatible with regulatory requirements. The brown University JAMA study and the CEPR report have documented the pattern of PE-backed ABA platforms prioritizing volume over clinical quality. When that prioritization produces supervision fraud, the question of sponsor liability becomes legally relevant under theories of corporate responsibility, respondeat superior, and in some jurisdictions, piercing the corporate veil.
The supervision fraud problem is not going to be solved by better documentation templates or AI auditing tools. It will be solved by BCBAs who refuse to sign off on sessions they did not observe, by clinical directors who set caseloads that allow meaningful supervision, by practice owners who prioritize clinical integrity over billable hour production, and by regulators who enforce supervision standards with the same rigor they apply to billing standards. Until those conditions exist, supervision fraud will remain the ABA industry’s most dangerous compliance gap.
AT A GLANCE
| Supervision requirement: | BCBAs must directly supervise RBTs at specified ratios and frequencies |
|---|---|
| Keller Grover findings: | Supervision fraud is one of the most common FCA violation categories in ABA |
| Common patterns: | Excessive caseloads, billing for absent supervision, cursory check-ins, forged signatures |
| MN criminal case: | 4M scheme; unqualified technicians; forged signatures; guilty plea March 2026 |
| MN investigations: | 85 open investigations; FBI raids Dec 2024; 90-day payment delays |
| MA Inspector General: | 7.3M overpayments driven partly by inadequate supervision ratios |
| OIG audit findings: | Supervision deficiencies found in all 4 states audited |
| FCA whistleblower awards: | 15–30% of government recovery |
| Liability chain: | Individual BCBA → clinical director → practice owner → PE sponsor |
SOURCES & REFERENCES
| 1. | Keller Grover. “False Claims Act Violations in ABA Therapy Treatment for Autism.” January 28, 2026. |
|---|---|
| 2. | Sanford Heisler Sharp. “Fraud Against Autistic Individuals, Their Loved Ones, and Beyond.” December 29, 2025. |
| 3. | Benesch. “Heightened Scrutiny of Medicaid-Funded ABA Services.” March 2026. |
| 4. | Benesch. “OIG Finds Significant Improper Medicaid Payments for ABA in WI and IN.” January 2026. (MA 7.3M.) |
| 5. | HHS-OIG. Indiana, Wisconsin, Maine, Colorado audit reports. 2024–2026. |
| 6. | Whistleblower Law Collaborative. “Medicaid Fraud Risks in ABA Therapy.” March 2026. (MN criminal case.) |
| 7. | KFF Health News. “Oz escalates Medicaid fraud claims.” March 2026. (MN 85 open investigations; FBI raids.) |