Five Years, Three Divestitures, One Sale at a Loss
FRISCO, TEXAS — Centene Corporation bought Magellan Health in January 2022 for $2.2 billion. The deal was supposed to give the country’s largest Medicaid managed care organization a specialized behavioral health engine. What it gave Centene instead was an accelerating cost problem it spent the next four years trying to manage.
The stripping began immediately. In December 2022, Centene sold Magellan Rx, the pharmacy benefit management business, to Prime Therapeutics for $1.35 billion. In January 2023, it sold Magellan Specialty Health, the radiology and musculoskeletal benefit management arm also known as NIA, to Evolent Health for approximately $660 million. Those two sales recovered a combined $2 billion from the original acquisition price before a dollar of behavioral health value was returned.
What remained after those divestitures was the piece Centene originally needed most: the core managed behavioral health business. Carve-out contracts with health plans, employers, and government agencies. Behavioral health authorization and utilization management. Crisis services. And, prominently, the autism care program now managed under the Magellan Autism Connections brand.
By December 2025, Centene had signed a definitive agreement to sell that remaining business as well. On February 6, 2026, Centene disclosed the agreement in its year-end financial results without naming the buyer. A week later, on February 13, Magellan announced via LinkedIn that the buyer was Madison Health Group, a relatively new investment and innovation firm focused on behavioral health. Financial terms of the transaction were not disclosed. What Centene did disclose was the damage: a recognized financial loss of $513 million, or $389 million after taxes, on the sale of the asset it had paid $2.2 billion to acquire.
CEO Caroline Carney, MD, will continue to lead Magellan following the close. The transaction remains subject to customary closing conditions and regulatory approvals as of this writing.
“Behavioral health was the most significant driver of the quarter-over-quarter increase with ABA, or applied behavioral analysis, as an accelerating pressure point across a number of our markets.” — Centene CEO Sarah London, Q2 2025 earnings call
Why Centene Sold: The ABA Cost Problem
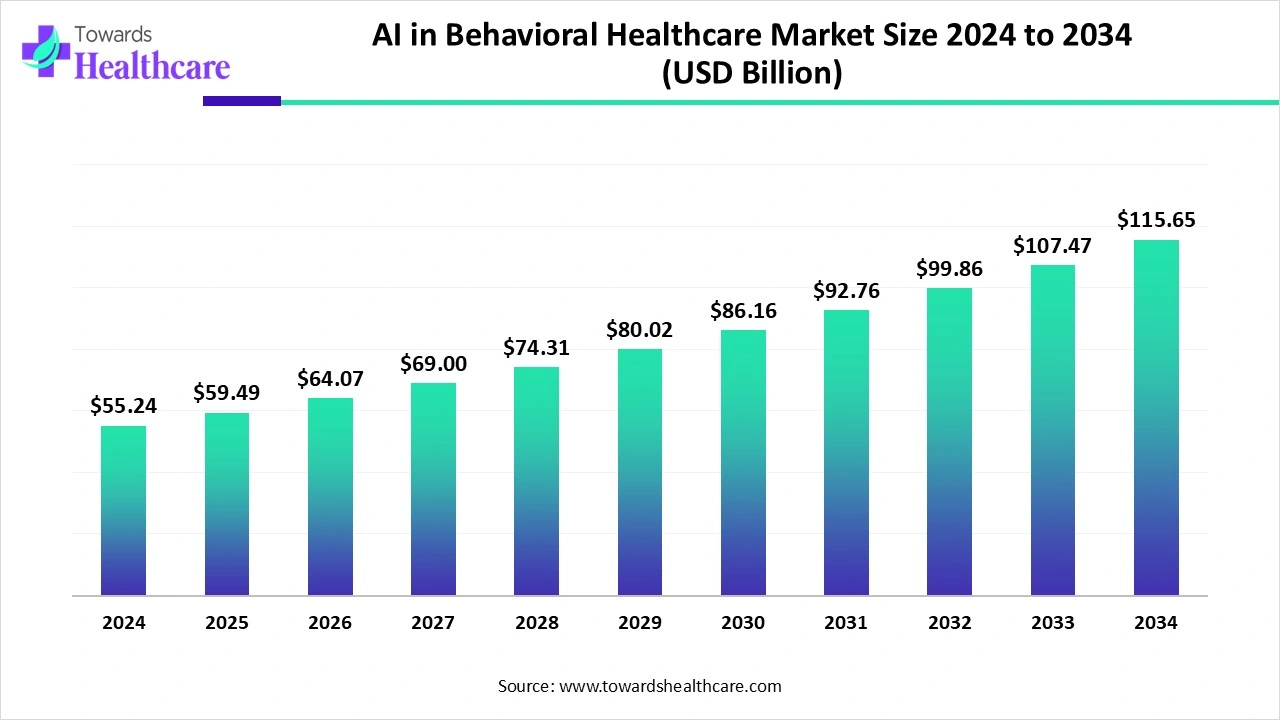
Centene did not hide its reasoning. Across multiple earnings calls, its chief executives connected behavioral health broadly and ABA specifically to cost outcomes that fell outside their financial models. In a Q2 2025 earnings call, CEO Sarah London named ABA by acronym as “an accelerating pressure point across a number of our markets.” In its Q4 2025 earnings call, Centene disclosed that behavioral health accounted for roughly half of the company’s excess costs. The company assembled a dedicated task force to examine ABA spending.
The problem is structural to how large insurance organizations interact with ABA therapy. ABA is an intensive, time-based service that can run from several hours to 40-plus hours per week for a single member. Authorization management, network adequacy, quality monitoring, and utilization review for ABA require specialized clinical expertise that most health plans do not build internally. Plans that underinvest in that clinical infrastructure tend to see high unit costs, high authorization rates, and wide variability in outcomes. Those problems compound as autism diagnoses grow.
Centene is not the only player that has felt this pressure. But I experienced it at scale. Its Medicaid book is among the country’s largest, and Medicaid is the primary payer for ABA in most states. As state Medicaid agencies have struggled with ABA cost trajectories, as described by the Indiana reform package and the Wisconsin OIG findings elsewhere in this issue, the managed care plans that carry that Medicaid risk have felt the same pressure expressed in different forms: as excess costs on their income statements.
The decision to sell Magellan at a loss rather than continue absorbing behavioral health cost pressure signals something specific about how at least one large payer has reassessed the vertical integration thesis for managed behavioral healthcare. Centene bought Magellan in part to bring behavioral health expertise inside the organization. The bet did not pay off on the terms Centene needed it to. Whether that reflects a problem with the ABA category specifically, with the carve-out model generally, or with Centene’s particular execution is not yet clear from public disclosures.
What Magellan’s ABA Program Actually Is
Before examining what the ownership change means for ABA providers, it is worth being precise about what Magellan’s ABA business consists of. The Magellan Autism Connections program is not a provider of ABA therapy. It is a manager and administrator of ABA benefits for health plans, employers, and government agencies that contract with Magellan for behavioral health carve-out services.
In 2025, the Autism Connections program managed ABA services for more than 12,000 members. The clinical team supporting the program included 46 specialized staff, approximately 40 of whom are behavior analysts. The program’s clinical philosophy, as described by its medical director, centers on what the company calls “care shaping” rather than traditional utilization management. The stated goal is to minimize denials and maximize engagement with providers, with cost containment focused on outcomes quality and appropriate intensity rather than authorization restrictions.
The cost data Magellan has published for its program is striking. Unmanaged ABA, according to Magellan’s internal data, costs between $125,000 and $300,000 per member annually. ABA managed by other organizations typically runs between $40,000 and $60,000 per member. Magellan’s managed ABA averages $29,161 per member. The company has also published outcome data: 88% of members make excellent clinical progress at a cost below $24,000 annually, 75% achieve substantial developmental progress on Vineland adaptive behavior scores, and members demonstrate a 54% improvement in social behaviors and a 58% improvement in behavioral domains on standardized assessment. Magellan has also been first to market with value-based contracting arrangements with ABA providers, through partnerships with organizations including Kyo Autism Therapy.
Magellan’s overall behavioral health network includes more than 118,000 credentialed providers. Its ABA contracts cover both in-network service delivery and, in limited circumstances, single-case agreements for members in low-density markets or with complex clinical needs that no in-network provider can serve. The out-of-network utilization rate in a large Magellan-managed plan was 1.2% in a recent reported period, which is among the lower rates in the industry.
The program also serves several categories outside commercial insurance: services for foster children, crisis behavioral health services, behavioral health prescribing management, complex and high-acuity cases, and services to active-duty military and federal agencies. That last category represents the TRICARE-adjacent and federal employee benefit program work that is part of Magellan’s government-facing book. Magellan also manages behavioral health for multiple state Medicaid programs through carved-out contracts.
Unmanaged ABA costs between $125,000 and $300,000 per member annually. ABA managed by other organizations costs $40,000 to $60,000. Magellan’s managed ABA averages $29,161 per member. Those numbers are Magellan’s own, but they explain why the carve-out contract has value to payers who are serious about behavioral health cost management.
Madison Health Group and the Independence Thesis

Madison Health Group describes itself as an investment and innovation firm focused on whole-person care, expanded access to care, innovative technologies, artificial intelligence, data analytics, and clinical quality. Its advisory board includes Christina Mainelli, former CEO of Quartet Health, a digital behavioral health platform; Christopher Molaro, current CEO of NeuroFlow, a platform for behavioral health integration and monitoring; and Kenneth Fasola, a former president at Centene Corporation itself. The last name on that list carries weight in the context of the deal: a former Centene executive is among the advisors backing the firm that is buying Magellan from Centene.
In its LinkedIn announcement of the transaction, MHG stated that Magellan would become “the only independent, managed behavioral healthcare company focused exclusively on providing access to quality care to communities domestically and abroad.” The “only independent” framing is an explicit competitive positioning claim. The major managed behavioral health organizations in the United States either operate as subsidiaries of large insurance companies, as Magellan did under Centene, or as captive carve-out vendors closely integrated with specific health plan relationships. An independent Magellan would theoretically be able to contract with any health plan, including plans that compete with Centene, without organizational conflict.
MHG said that Magellan’s evidence-based clinical programs, including carve-out services, autism care, crisis services, foster care services, behavioral health prescribing, complex and high-acuity management, and services to active-duty military and federal agencies, will remain in place. If the deal closes, Magellan plans to expand those programs into new markets with enhanced technology, AI, data, and analytical solutions. The specific technology roadmap has not been disclosed. Based on the advisory board’s backgrounds in digital behavioral health, the strategic direction is likely to involve greater data infrastructure, predictive analytics, and possibly remote monitoring capabilities for behavioral health management.
What MHG is paying for the asset is unknown. The absence of disclosed financial terms is consistent with private transactions of this type, but it makes it difficult to assess whether MHG is acquiring Magellan as a turnaround play, a growth platform, or a strategic asset to be integrated with existing portfolio companies. The advisory board’s behavioral health technology orientation suggests the bet is on technology-enabled cost management and clinical quality improvement rather than on traditional carve-out expansion.
What This Means for ABA Providers Under Magellan Contracts
For ABA providers that currently hold Magellan contracts, the ownership change has several practical implications worth tracking, even before the deal closes.
Contract continuity in the near term. Magellan’s carve-out contracts are held by Magellan Health, not by Centene directly. The sale of Magellan’s equity to MHG does not automatically trigger assignment or renegotiation clauses in provider contracts. In most standard managed care contract structures, a change of ownership that results in the contracted entity continuing operations under the same legal structure does not constitute a material change requiring provider consent. Caroline Carney continuing as CEO reinforces the operational continuity message. Providers should review their specific contract terms, particularly any change-of-control or assignment provisions, and monitor for any notices from Magellan about contract amendments post-close.
The independence upside. An independent Magellan has more latitude to expand its contracted footprint. Under Centene, Magellan’s carve-out relationships were primarily with health plans that Centene was not competing with, or were internal to Centene’s managed care business. Free from that constraint, Magellan can approach any health plan in the country as a potential carve-out customer. For ABA providers, more markets covered by Magellan’s managed network potentially means more Magellan contracts to hold, more Magellan prior authorizations to navigate, and more Magellan rate structures to negotiate.
The technology direction. MHG’s advisory board is stacked with digital behavioral health backgrounds. NeuroFlow specifically works on behavioral health integration and monitoring within medical care settings. Quartet Health built a platform for connecting patients to behavioral health care. Both are data-intensive, analytics-driven approaches to behavioral health management. If Magellan’s ABA program moves in the direction suggested by its new backers, it may deploy more sophisticated monitoring of clinical outcomes, more granular utilization review, or AI-assisted prior authorization processes. For well-run ABA providers that document outcomes rigorously, that direction is potentially favorable. For providers who rely on thin documentation, it creates new risk.
The Idaho warning. When Idaho’s Department of Health and Welfare removed ABA from Magellan’s managed behavioral health contract in late 2025, moving it instead to a state-managed fee-for-service schedule under different billing codes, the disruption for ABA providers was immediate. CPT codes used for ABA authorization and billing were replaced by Healthcare Common Procedure Coding System codes under the new program. Concurrent billing was eliminated. Revenue cycle management processes built around Magellan’s authorization system became obsolete overnight. That example illustrates the dependency risk that comes with having a significant portion of a clinic’s Medicaid-covered clients under a single managed care contractor. Market-level events outside individual provider control can reshape billing rules with minimal notice.
The Magellan-to-Madison transition is not an Idaho scenario. The clinical programs are stated to remain in place, and MHG is betting on Magellan’s growth rather than its contraction. But it is a reminder that managed behavioral health carve-out relationships are subject to ownership changes, strategic pivots, and re-contracting events that sit entirely outside the provider’s influence. Diversification of payer relationships, documentation quality, and outcomes measurement are the variables providers can control when the payer side of the equation changes.
The Broader Signal: Payers Reassessing Behavioral Health Assets
Centene’s decision to sell Magellan at a loss is not an isolated data point. It reflects a pattern that has been visible across the managed care industry for the past two years: large insurance organizations that made behavioral health acquisitions in the post-pandemic period are now reassessing those assets as behavioral health costs prove more difficult to manage than anticipated.
The core challenge is that ABA in particular does not behave like most medical benefits under managed care. The utilization drivers are clinical and developmental, not primarily acute or episode-based. A child in ABA therapy may be authorized for 20 hours per week for several years. The authorization volume is predictable, the clinical logic for the hours is defensible, and the cost is real and sustained. Standard utilization management tools designed for acute medical care do not translate cleanly to that cost structure.
Magellan’s managed ABA model represents one approach to that problem: specialized clinical teams, outcomes-focused authorization, and value-based contracting with providers. Whether that model proves sustainable as an independent business with technology investment from MHG is a question the industry will be watching. If Magellan can demonstrate that managed behavioral health carve-outs generate better outcomes and lower costs than the integrated model Centene tried, the independence thesis may attract other health plans looking to offload behavioral health risk. If Magellan struggles to grow its contracted footprint, or if the technology investment thesis does not reduce per-member costs, a future divestiture or merger becomes more likely.
For ABA providers, the outcome of the Madison Health Group bet matters because Magellan’s managed care infrastructure touches a significant portion of the commercial ABA market and several state Medicaid programs. The clinical and financial terms under which ABA is authorized, reimbursed, and quality-monitored in those markets will be shaped, at least in part, by what kind of company Magellan becomes under new ownership.
AT A GLANCE
| Original deal: | Centene acquired Magellan Health for $2.2 billion; closed January 2022 |
|---|---|
| Prior divestitures: | Magellan Rx sold to Prime Therapeutics for $1.35B (December 2022); Magellan Specialty Health (NIA) sold to Evolent Health for ~$660M (January 2023) |
| MHG deal announced: | February 13, 2026 (LinkedIn); Centene disclosed in year-end results February 6, 2026 without naming buyer |
| Definitive agreement signed: | December 2025 |
| Financial terms: | Not disclosed |
| Centene recognized loss: | $513 million ($389 million after taxes) |
| Magellan CEO: | Caroline Carney, MD (continuing) |
| MHG advisors: | Christina Mainelli (former Quartet CEO); Christopher Molaro (NeuroFlow CEO); Kenneth Fasola (former Centene president) |
| MHG positioning: | “The only independent, managed behavioral healthcare company focused exclusively on providing access to quality care” |
| Programs retained: | Carve-out services, autism care, crisis services, foster care, behavioral health prescribing, complex/high-acuity management, active-duty military and federal agencies |
| ABA program scale (2025): | 12,000+ members; 46-person specialized team including ~40 behavior analysts |
| Magellan ABA cost per member: | $29,161 average vs. $40,000-$60,000 (industry managed) vs. $125,000-$300,000 (unmanaged) |
| Clinical outcomes claimed: | 88% make excellent progress under $24K/year; 75% Vineland developmental progress; 54%/58% social/behavioral domain improvement |
| Why Centene sold: | Behavioral health = ~50% of excess costs (Q4 2025 earnings); ABA cited as “accelerating pressure point” (Q2 2025 earnings); dedicated ABA task force formed |
| Closing conditions: | Customary regulatory approvals required; not yet closed as of April 2026 |
SOURCES & REFERENCES
| 1. | Becker’s Behavioral Health. “4 Behavioral Healthcare M&A Deals in 2026.” March 9, 2026. https://www.beckersbehavioralhealth.com/behavioral-health-capital-investment/3-behavioral-healthcare-ma-deals-in-2026/ |
|---|---|
| 2. | Becker’s Payer Issues. “Centene’s Magellan Health to Be Acquired by Investment Group.” February 18, 2026. https://www.beckerspayer.com/m-and-a/magellan-health-to-be-acquired-by-investment-group/ |
| 3. | Becker’s Behavioral Health. “Magellan Health to Be Acquired by Investment Group.” February 17, 2026. https://www.beckersbehavioralhealth.com/behavioral-health-capital-investment/magellan-health-to-be-acquired-by-investment-group/ |
| 4. | Lovett, Laura. “Magellan Health to Become Independent Again Under Madison Health Group Deal.” Behavioral Health Business. February 17, 2026. https://bhbusiness.com/2026/02/17/magellan-health-to-become-independent-again-under-madison-health-group-deal/ |
| 5. | Lovett, Laura. “Centene Is Ready to Sell Magellan, Even if It Comes at a Loss.” Behavioral Health Business. February 20, 2026. https://bhbusiness.com/2026/02/20/centene-is-ready-to-sell-magellan-even-if-it-comes-at-a-loss/ |
| 6. | OPEN MINDS (via PA Providers). “Magellan Health Announces Sale Agreement With Madison Health Group.” February 18, 2026. https://paproviders.org/wp-content/uploads/2026/02/Magellan-Sale-OPEN-MINDS-Weekly-News-Wire.pdf |
| 7. | Becker’s Behavioral Health. “Why Magellan Bets on Clinical Expertise, Provider Partnerships in Autism Care.” April 2026. https://www.beckersbehavioralhealth.com/autism-care/why-magellan-bets-on-clinical-expertise-provider-partnerships-in-autism-care/ |
| 8. | Magellan Healthcare. “Magellan Autism Connections.” magellanhealthcare.com. Accessed April 2026. https://www.magellanhealthcare.com/health-plans/autism-connections/ |
| 9. | Behavioral Health Business. “Why Most Payers, Providers Abhor Out-of-Network Billing in Autism Therapy.” October 15, 2025. https://bhbusiness.com/2025/10/15/why-most-payers-providers-abhor-out-of-network-billing-in-autism-therapy/ |
| 10. | Behavioral Health Business. “What Happens When ABA Is Moved Out of Medical Coverage.” January 12, 2026. https://bhbusiness.com/2026/01/12/what-taking-aba-out-of-medical-benefits-could-mean-for-idaho-and-beyond/ |
| 11. | Behavioral Health Business. “Idaho’s Reclassification of Autism Therapy Could Rattle ABA Reimbursement.” November 10, 2025. https://bhbusiness.com/2025/11/10/idahos-reclassification-of-autism-therapy-could-rattle-aba-reimbursement/ |
| 12. | Centene Corporation. “Centene Completes Divestiture of Magellan Rx.” Press release. December 5, 2022. https://www.prnewswire.com/news-releases/centene-completes-divestiture-of-magellan-rx-301694373.html |
| 13. | Centene Corporation. “Centene Completes Divestiture of Magellan Specialty Health.” Press release. January 23, 2023. https://investors.centene.com/2023-01-23-CENTENE-COMPLETES-DIVESTITURE-OF-MAGELLAN-SPECIALTY-HEALTH |
| 14. | Mission Viewpoint. “MissionViewpoint Monthly Update, March 2026.” https://www.missionviewpoint.com/missionviewpoint-monthly-update-march-2026/ |









Join the discussion ▾