Deal Volume Is Up. Valuations Are Down. What Explains the Gap?
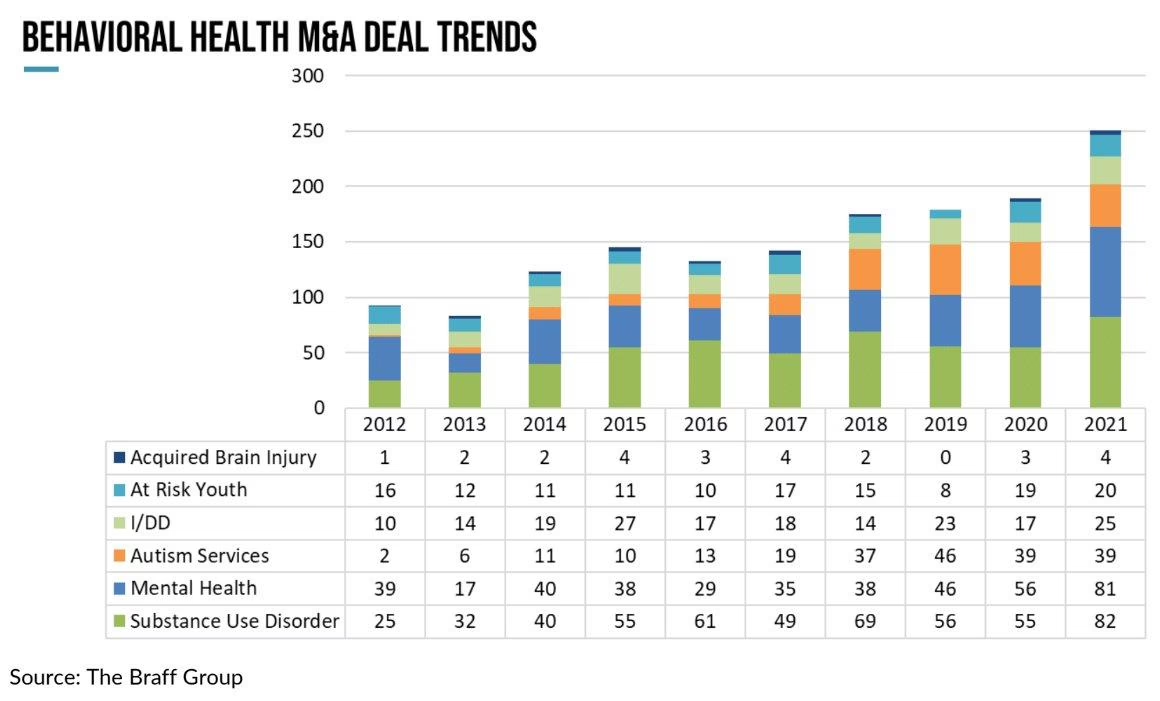
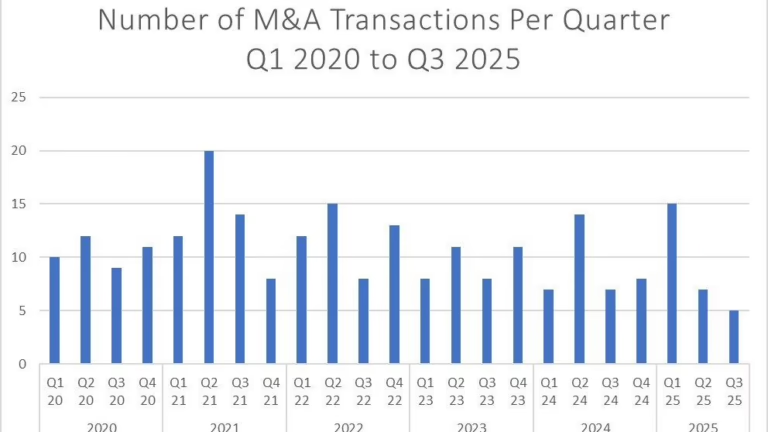
ACROSS THE UNITED STATES — the ABA mergers and acquisitions market is sending two signals simultaneously, and they appear to contradict each other. Deal volume has returned to its strongest levels since 2021, with Mertz Taggart reporting 47 behavioral health transactions in Q1 2025 alone — including 34 M&A deals, the highest quarterly count since Q4 2022. Autism and I/DD transactions specifically reached 12 deals in Q1 2025, the highest volume since 2021. Yet at the same time, the EBITDA multiples that buyers are willing to pay for ABA providers have compressed noticeably from the peaks of 2021 and early 2022.
The compression is most visible in the middle of the market. Platform-level ABA transactions — providers with 50 or more locations, diversified payer relationships, and audited financials — still command multiples in the 12x to 15x EBITDA range, according to FOCUS Investment Banking’s 2025 behavioral health multiples analysis. The 2024 sale of Behavioral Innovations for approximately $300 million at roughly 15x EBITDA illustrates the premium that scaled platforms continue to attract. But below that tier, the picture has shifted. ABA practices in the $3 million to $10 million EBITDA range are increasingly trading at 6x to 8x EBITDA, down from the 8x to 12x range that characterized the 2020–2022 peak.
For ABA practice owners, this compression creates a specific strategic problem. The demand signal — PE firms actively seeking ABA acquisitions, deal volume at multi-year highs — suggests a strong seller’s market. But the pricing signal tells a different story: buyers are applying larger risk discounts, conducting more rigorous due diligence, and walking away from deals that would have closed with less scrutiny two years ago. Understanding what is driving this gap is essential for any practice owner who is considering a sale or recapitalization in the current market.
The ABA M&A market has bifurcated: scaled platforms with clean financials, diversified payers, and demonstrable clinical governance still command premium multiples, while smaller providers face a valuation environment shaped by fraud headlines, Medicaid uncertainty, and heightened buyer scrutiny.
Factor One: Fraud and Audit Headlines Have Changed Buyer Risk Perception
The single largest driver of ABA valuation compression is the cumulative effect of fraud investigations, billing audits, and compliance actions that have generated persistent negative headlines across the sector since 2022. High-profile cases — including OIG Medicaid audits in multiple states, False Claims Act whistleblower lawsuits, and criminal indictments against individual ABA providers — have not only damaged the reputations of the specific organizations involved but have altered how every buyer evaluates every ABA acquisition target.
The mechanism is straightforward. When a PE firm’s investment committee reviews an ABA acquisition opportunity, the first question is no longer about growth potential or market share — it is about compliance risk. Has the target been audited? Are its billing practices defensible? Does it have a compliance program that would withstand regulatory scrutiny? Is there any whistleblower exposure? These questions were always part of healthcare services due diligence, but the frequency and severity of ABA-specific enforcement actions have elevated compliance from a checklist item to a threshold issue. A target that cannot satisfactorily address compliance concerns does not advance to pricing discussions.
The practical effect on valuations is significant. Buyers are applying larger compliance-related risk discounts to their EBITDA calculations, adjusting for potential liability exposure, and in some cases reducing their offered multiples by one to two turns specifically to account for regulatory risk. For a practice with $5 million in EBITDA, a one-turn reduction in multiple represents a $5 million reduction in enterprise value. For a practice owner who expected to sell at 10x and receives offers at 8x, the difference is $10 million in personal wealth.
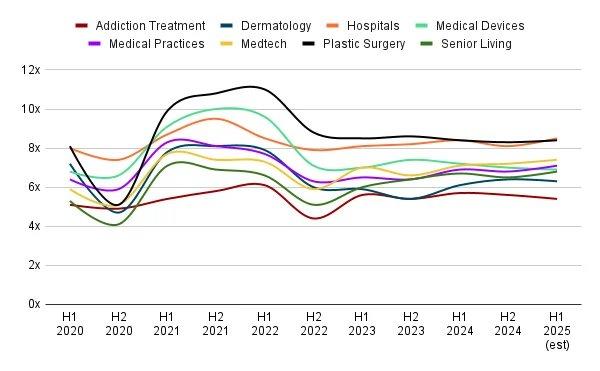
Factor Two: Medicaid Rate Instability and Payer Concentration Risk
ABA providers that derive a significant share of revenue from Medicaid are facing a second source of valuation pressure: uncertainty about future reimbursement rates. Medicaid rate cuts in several states, combined with broader federal budget discussions that could affect Medicaid funding levels, have introduced a degree of revenue uncertainty that directly affects how buyers model future cash flows.
The impact on valuations works through the discounted cash flow analysis that underlies every EBITDA multiple. When a buyer applies a multiple to a target’s EBITDA, that multiple implicitly reflects the buyer’s assessment of the durability and growth trajectory of those earnings. If Medicaid rates are expected to remain stable or increase, the multiple is higher. If rates are expected to decline or become unpredictable, the multiple compresses to account for the increased risk.
Payer concentration as a valuation discount: ABA providers that derive more than 50 percent of revenue from a single state’s Medicaid program face an additional concentration discount. Buyers view single-payer dependence as a structural risk — if that state cuts rates or changes coverage criteria, the financial impact is immediate and difficult to offset. Providers with diversified payer relationships across commercial insurance, multiple state Medicaid programs, and private pay command higher multiples specifically because their revenue base is more resilient to any single payer’s actions.
The providers that command premium valuations in the current market share several characteristics: they operate across multiple states, they have a balanced mix of commercial and Medicaid payers, they hold national accreditation, and they can demonstrate measurable clinical outcomes. These attributes reduce buyer risk and support higher multiples. Providers that lack one or more of these characteristics face correspondingly larger discounts.
Factor Three: Post-COVID Margin Compression and the Wage-Rate Squeeze
The third major factor behind ABA valuation compression is a structural margin problem that emerged during and after the COVID-19 pandemic. ABA providers experienced significant wage inflation as competition for Board Certified Behavior Analysts and Registered Behavior Technicians intensified. At the same time, many providers were unable to secure corresponding rate increases from payers, particularly Medicaid programs. The result was a sustained compression of operating margins that reduced the EBITDA available for valuation.
Mertz Taggart managing partner Kevin Taggart described this dynamic directly: during COVID and immediately afterward, many ABA companies experienced wage inflation without receiving rate increases. Several high-profile ABA providers subsequently exited state markets or filed for bankruptcy, including exits from California, Colorado, and other states. These failures created a cautionary precedent that has made buyers more conservative in their margin assumptions when evaluating ABA targets.
When buyers model ABA acquisitions in 2025 and 2026, they are not using the margin profiles of 2019 or 2020. They are using the compressed margins of 2023 and 2024 — and in many cases applying additional haircuts to account for continued wage pressure and uncertain rate environments.
The practical consequence for practice owners is that EBITDA itself — the numerator in the valuation equation — has declined for many ABA providers. When a lower EBITDA is multiplied by a lower multiple, the compounding effect on enterprise value can be substantial. A practice that generated $8 million in EBITDA at 10x in 2021 (an $80 million valuation) might now generate $6 million in EBITDA at 7x (a $42 million valuation). That represents a 47 percent decline in enterprise value, even though the practice is still profitable and growing revenue.
What This Means for Practice Owners Considering a Sale
The ABA valuation compression does not mean the M&A market is closed. To the contrary, deal volume is strong and buyer interest remains robust. What has changed is the pricing environment — and the specific characteristics that differentiate practices that command premium multiples from those that receive discounted offers.
Practices that will achieve the best outcomes in the current environment share several attributes. They have clean compliance histories with documented billing programs and internal audit processes. They operate across multiple payer types and preferably multiple states. They have strong BCBA retention rates and can demonstrate clinical outcome data. They have professionalized their financial reporting with audited or reviewed financial statements. And they have addressed the margin compression problem through some combination of rate negotiations, service mix optimization, and operational efficiency improvements.
Practices that will face the most challenging valuations are those with concentrated Medicaid revenue in a single state, thin or declining margins, limited compliance infrastructure, high staff turnover, and financial statements that require significant normalization. These practices may still find buyers, but the offers they receive will reflect the full weight of the risk factors described in this article.
For the ABA industry as a whole, the valuation compression represents a maturation of the market. The period from 2018 to 2022, when almost any ABA practice with positive EBITDA could attract PE interest at attractive multiples, was an anomaly driven by a surge of capital entering a newly discovered sector. The current environment — high deal volume, differentiated pricing, rigorous due diligence, and compliance-first evaluation — is what a mature healthcare services M&A market looks like. Practice owners who understand this shift and prepare accordingly will be better positioned to achieve their transaction objectives.
AT A GLANCE
| Q1 2025 deal volume: | 47 behavioral health transactions; 34 M&A deals (Mertz Taggart) |
|---|---|
| Autism/I/DD Q1 2025: | 12 deals — highest volume since 2021 (Mertz Taggart) |
| Platform multiples (2025): | 12x–15x EBITDA for scaled, multi-state platforms (FOCUS Investment Banking) |
| Mid-market multiples: | 6x–8x EBITDA for ABA practices in the $3M–$10M EBITDA range |
| Peak-era multiples: | 8x–12x EBITDA (2020–2022 for mid-market ABA providers) |
| Benchmark deal: | Behavioral Innovations sold for ~$300M at ~15x EBITDA (2024) |
| Compression driver #1: | Fraud/audit headlines and heightened compliance due diligence |
| Compression driver #2: | Medicaid rate instability and payer concentration risk |
| Compression driver #3: | Post-COVID wage inflation without corresponding rate increases |
| Premium differentiators: | Multi-state footprint, diversified payers, clinical outcomes data, clean compliance |
SOURCES & REFERENCES
| 1. | Mertz Taggart. “Q1 2025 Behavioral Health M&A Report.” 2025. |
|---|---|
| 2. | FOCUS Investment Banking. “Behavioral Health EBITDA Multiples 2025 Update.” December 2025. |
| 3. | Scope Research and PitchBook. Behavioral health transaction data cited in FOCUS Investment Banking analysis. 2025. |
| 4. | Mergium Advisors. “Valuation EBITDA Multiples for Autism Practices and Pediatric Therapy Businesses.” October 2025. |
| 5. | MA Healthcare Advisors. “Behavioral M&A Trends: Insights on 2025 Market Shifts.” March 2025. |
| 6. | Behavioral Health Business. Various ABA transaction reports. 2024–2026. |