The ACES Breakthrough
On August 1, 2021, Aetna, a CVS Health company, and ACES announced an enhanced relationship that would change the trajectory of value-based care in ABA. Through a new national agreement, Aetna members gained access to value-based autism care from ACES clinical providers. The companies also created Aetna’s first Applied Behavioral Analysis Institute of Quality — a designation that recognizes facilities offering specialized clinical services that meet standards of quality and cost efficiency.
Kristin Farmer, founder and CEO of ACES, described the designation as confirming ACES as a leading care model for the autism community. Cara McNulty, then President of Behavioral Health and Employee Assistance at Aetna, called the collaboration a key part of Aetna’s commitment to improving access to quality mental health care, noting that ACES’s clinical care model for ABA is industry-leading. Angie Meoli, SVP of Network Strategy and Provider Experience at Aetna, framed the arrangement as delivering a differentiated provider network that is consumer-focused, supported by a value-based arrangement that keeps care focused on patient outcomes and affordability.
The IOQ designation is significant beyond ACES because it establishes a template for how payers can create tiered provider networks in ABA. The designation recognizes providers based on excellence in care, commitment to continuous improvement, and ability to meet certain standards of quality and cost efficiency. For payers, this creates a mechanism to steer members toward high-performing providers. For providers, it creates a competitive advantage that cannot be replicated simply by opening more locations or billing more hours.
ACES’ IOQ locations span multiple states including North Carolina, Oklahoma, Texas, Utah, and Washington. The Aetna IOQ page confirms that ACES is the first provider group to be named an ABA Institute of Quality. The national scope of the designation gives ACES a competitive moat in Aetna’s network that no other ABA provider has matched in the five years since the agreement was announced.
Forbes named ACES one of America’s Best Midsize Employers, and the company publishes comprehensive quality index measures including client outcome data, payer audit results, and treatment planning metrics. The transparency of outcomes reporting is a prerequisite for value-based contracting: payers will not link payment to outcomes they cannot measure, and providers that cannot demonstrate outcomes will not qualify for VBC arrangements.
Our collaboration with ACES on Aetna’s first-ever autism Institute of Quality is a key part of our commitment to improving access to quality mental health care. The quality and effectiveness of ACES’ clinical care model for ABA is industry-leading. — Cara McNulty, President, Behavioral Health, Aetna
What VBC Demands From Technology
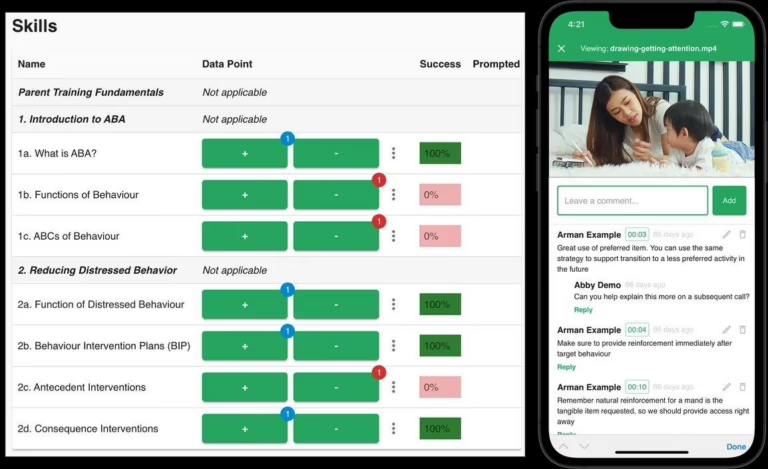
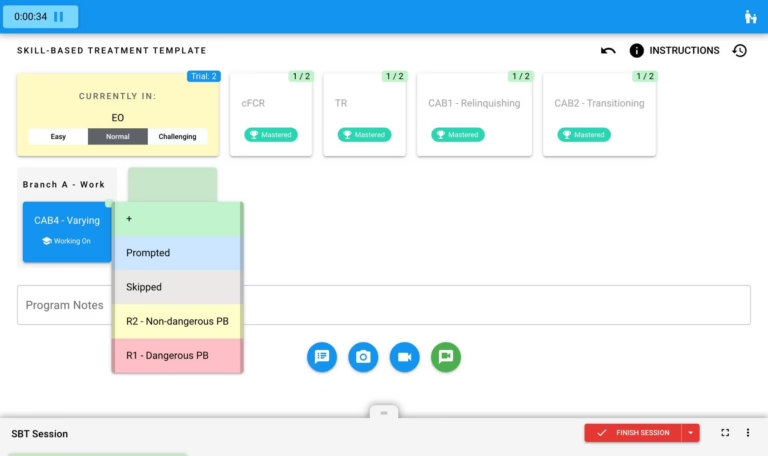
Value-based care requires a fundamentally different technology stack than fee-for-service billing. In FFS, the technology’s primary function is to submit claims accurately and get paid for hours delivered. In VBC, the technology must measure clinical outcomes, track treatment progress against benchmarks, report outcomes to payers in standardized formats, identify clients who are not progressing and trigger clinical interventions, and provide population-level analytics that demonstrate the provider’s aggregate clinical effectiveness.
A 2025 paper in Behavioral Sciences, published in a special issue on early identification and intervention of autism, examined the implications of value-based care for autism services. The authors noted that fee-for-service payment systems create incentives to increase clinical volume that often work in opposition to efforts to coordinate care or improve care delivery. Value-based care shifts the focus from generating volume toward providing more efficient, coordinated care. But the paper also identified a critical challenge: the absence of standardized autism-specific care quality metrics.
The paper argued that norm-referenced measures often do not meaningfully inform treatment goals or quantify progress, and that because many intensive service providers like behavior analysts are not trained in administering these measures, families are often required to seek out specialists for re-evaluation, adding to the access bottleneck. The authors called for meaningful autism-specific care quality metrics developed collaboratively among experts in autism services and psychometrics, autistic people and their families, and payers.
This metrics gap is the central technology challenge of VBC in ABA. The industry does not have a consensus set of outcome measures that payers, providers, and families all agree are meaningful, measurable, and comparable across providers. Without such measures, VBC contracts must rely on process metrics like documentation completeness or utilization rates rather than true outcome metrics like skill acquisition rates or functional independence gains.
CentralReach and AI.Measures
CentralReach’s exclusive partnership with AI.Measures represents the most significant technology investment in VBC readiness in the ABA market. The partnership was announced with the explicit goal of transforming the way assessments and autism care are delivered, paving the way for improved learner outcomes and provider-driven value-based care. The collaboration aims to create standardized assessment tools that can generate the outcome data VBC contracts require.
CentralReach’s position as the dominant ABA platform, serving 4,000 practices with over 200,000 professionals, gives the AI.Measures partnership immediate scale. If the partnership produces assessment tools that become industry standards, CentralReach would become the de facto data infrastructure for VBC in ABA — a position that would be extremely difficult for competitors to challenge.
The partnership also reflects a strategic evolution for CentralReach from a practice management and billing platform to a clinical outcomes infrastructure. The company’s AI suite — cari, trained on over a billion data points — already includes clinical analytics capabilities. The AI.Measures partnership extends those capabilities into standardized assessments, creating a full-stack outcomes measurement system that can serve both provider-side clinical decision-making and payer-side outcomes reporting.
Hi Rasmus HiQ Impact Score
Hi Rasmus’s HiQ Impact Score offers an alternative approach to outcomes measurement. The framework combines access metrics, clinical quality indicators, and user experience data into one unified strategic signal designed for leaders navigating the shift to value-based care. The HiQ framework draws from global healthcare and data science methodologies, bringing together approaches that have been validated in other clinical domains and adapting them for ABA.
At the CASP conference, Hi Rasmus presented data demonstrating the HiQ framework’s ability to surface clinically meaningful differences across organizations of different sizes and contexts. One organization reached 58 million learning opportunities in Q1 2025; another drove high outcomes in underserved areas despite a modest client base. The key insight: impact is not about size but alignment. This framing positions HiQ as a tool for demonstrating clinical value regardless of organizational scale, making it relevant for both large platforms and small practices pursuing VBC.
The HiQ approach differs from CentralReach’s AI.Measures partnership in that it is built natively within the Hi Rasmus platform rather than through an external partnership. This gives Hi Rasmus tighter integration between the outcomes framework and the clinical data collection tools that generate the underlying data. For practices already on Hi Rasmus, HiQ provides a built-in outcomes reporting capability that requires no additional integration or vendor relationships.
The Path Forward
The transition to value-based care in ABA will be gradual, uneven, and technology-dependent. ACES’ three national VBC agreements demonstrate that the model is viable, but ACES is one provider among thousands. Scaling VBC across the industry requires solving the metrics problem, building the technology infrastructure, training the workforce, and aligning payer incentives — each of which is a multi-year effort.
The technology platforms that solve the outcomes measurement challenge first will have a structural advantage in the VBC market. Providers using platforms with standardized outcomes reporting will be better positioned to negotiate VBC contracts. Payers will prefer to contract with providers who can demonstrate outcomes using tools they trust. The platform that becomes the industry standard for outcomes measurement will effectively become the infrastructure layer of value-based ABA.
For practice owners evaluating technology investments, the VBC trajectory has immediate implications. Platforms that capture rich clinical data — not just billing data — will be more valuable in a VBC environment than platforms optimized solely for claims management. The time to invest in clinical data infrastructure is before VBC contracts become widespread, not after. Practices that can demonstrate outcomes when payers come calling for VBC discussions will be the ones that secure favorable terms.
The Behavioral Sciences paper concluded that as payment systems shift, there is a unique opportunity to develop meaningful autism-specific care quality metrics that meet payer requirements. The technology companies building those metrics today — CentralReach through AI.Measures, Hi Rasmus through HiQ, and others yet to emerge — are laying the foundation for a transformation that could ultimately align the ABA industry’s financial incentives with its clinical mission for the first time.
AT A GLANCE
| ACES IOQ: | First ABA provider designated Aetna Institute of Quality (Aug 2021); 3 national VBC agreements |
|---|---|
| ACES CEO: | Kristin Farmer (founder) |
| Aetna IOQ states: | NC, OK, TX, UT, WA |
| VBC definition: | Payment linked to clinical outcomes rather than billable hours |
| Key technology gap: | No consensus standardized outcome measures for ABA across providers |
| CentralReach + AI.Measures: | Exclusive partnership for standardized assessments; provider-driven VBC |
| Hi Rasmus HiQ: | Impact Score combining access, quality, and experience; built natively in platform |
| Behavioral Sciences paper: | Oct 2025; called for collaborative autism-specific quality metrics; critiqued norm-referenced measures |
| FFS problem: | Incentivizes volume over coordination; uniform high-intensity billing patterns as audit red flag |
| Industry status: | ACES is only provider with national VBC; model viable but not scaled |
SOURCES & REFERENCES
| 1. | ACES Autism. “Institute of Quality for Autism.” blog.acesaba.com. August 2021. |
|---|---|
| 2. | Fierce Healthcare. “Aetna, ACES Team to Launch Institute of Quality for Autism Care.” August 31, 2021. |
| 3. | Healthcare Finance News. “Aetna, ACES Team to Launch IOQ.” September 1, 2021. |
| 4. | Aetna. “Institutes of Quality: ABA IOQ Locations.” aetna.com. |
| 5. | ACES Autism. “Comprehensive Quality Index Measures.” blog.acesaba.com. |
| 6. | CentralReach / AI.Measures. Partnership announcement. GlobeNewswire / ITNewsOnline. |
| 7. | Hi Rasmus. “How Technology Is Transforming Outcomes in ABA.” CASP conference. May 2025. |
| 8. | Behavioral Sciences. “Value-Based Care and ACOs: Implications for Early Autism Diagnosis.” 15(10), 1354. October 2025. |