LINCOLN, NE — On July 1, 2025, providers of applied behavior analysis therapy in Nebraska received a notice that would reshape the state’s Medicaid ABA landscape in thirty-one days. Effective August 1, the Nebraska Department of Health and Human Services was cutting reimbursement rates across the board — by 48% for the registered behavior technician sessions that constitute the bulk of ABA hours, 51% for parent training, 37% for BCBA supervision, and as much as 79% for certain group and assessment services. The state said it had no choice. Nebraska’s Medicaid ABA spending had grown from $4.6 million in 2020 to $85.6 million in 2024 — a 1,750% increase in four years, and what DHHS official Matthew Ahern described as the fastest increase he had seen in any single program across the agency.
What followed the August 1 cuts was exactly what providers and advocates had warned about and exactly what the state’s officials said they had managed for: disrupted services, a legislative hearing, an auditor’s report documenting billing problems, a near-exit by the state’s largest private ABA provider, a policy reversal by that same provider one week later, and a national spotlight on Nebraska as a test case for how — and how not — to address runaway ABA costs.
“All these kids that have Medicaid will have more difficulty having access to vital treatment that will help them become more independent. We’re either going to pay it on the front end, doing these therapies, or on the back end for care provision when you don’t gain skills through their ABA programs.”
— Cathy Martinez, President, Autism Family Network of Nebraska
A 1,750% SPENDING INCREASE IN FOUR YEARS
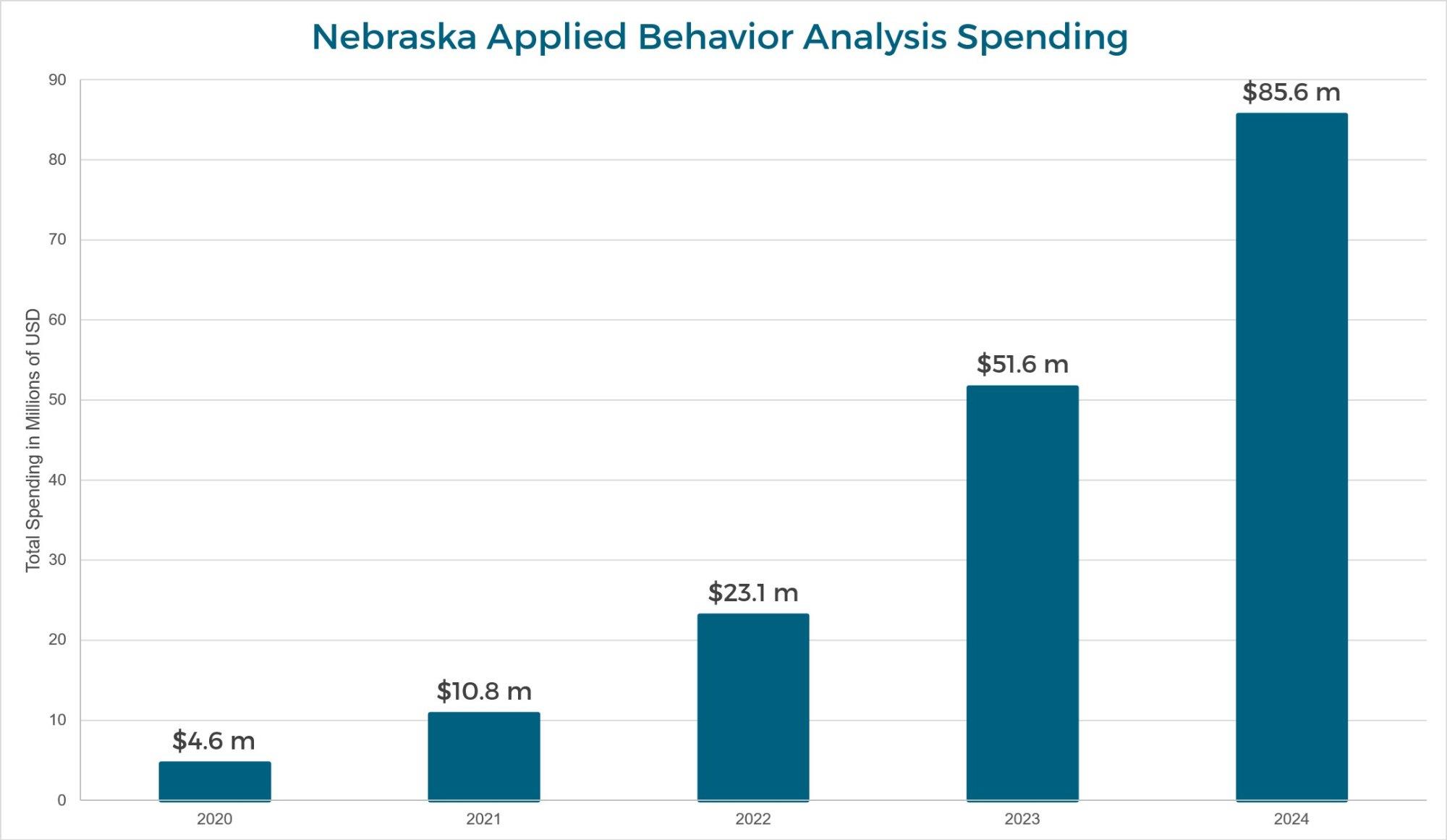
The numbers behind Nebraska’s rate cuts are stark. In 2020, Nebraska Medicaid spent $4.6 million covering ABA services for 169 children. By 2024, that figure had reached $85.6 million, serving roughly 1,500 families. The workforce had grown alongside it: roughly 459 certified behavioral health practitioners in 2020 expanded to more than 1,863 by 2024, and the number of BCBAs in Nebraska grew from approximately 100 to 356. What had been a niche program had, in the space of four years, become one of the fastest-growing line items in the state Medicaid budget.
DHHS said its review showed Nebraska had the highest ABA reimbursement rates of any state program. Drew Gonshorowski, the Division of Medicaid and Long-Term Care director who took office in December 2024, and DHHS CEO Steve Corsi were the public faces of that position. Corsi maintained that the rate adjustments were the result of a comparative analysis — benchmarked against neighboring states and against the Munroe-Meyer Institute’s analysis — and had been in the works well before the Trump administration’s federal Medicaid discussions. He said they had “zero” to do with state budget pressures.
That framing was challenged almost immediately. Providers noted that a 31-day notice period — the time between the July 1 announcement and the August 1 effective date — was insufficient to restructure business models, staffing levels, or contracts with managed care organizations. The Council of Autism Service Providers’ Mariel Fernandez, who would later testify at a legislative hearing, said she was genuinely surprised by how high some of Nebraska’s rates had gotten relative to surrounding states — but that the method of reduction was the problem, not the reduction itself.
THE RATE TABLE: WHAT CHANGED ON AUGUST 1
RBT direct therapy (97153) — Before: $36.11/unit · After: $18.70/unit · Change: −48%
BCBA supervision (97155) — Before: Higher · After: Reduced · Change: −37%
Parent training (97156) — Before: Higher · After: Reduced · Change: −51%
Treatment assessment — Before: Higher · After: Reduced · Change: −28%
Group / other services — Before: Higher · After: Reduced · Change: Up to −79%
The 48% cut to CPT code 97153 — RBT-delivered individual ABA therapy — was the most consequential by volume. That code alone represents the majority of billed ABA hours statewide and the majority of the program’s cost. A cut that large, applied with one month’s notice, had an immediate effect on provider math. For Above and Beyond Therapy, the largest private ABA provider in Nebraska, the calculation was blunt: DHHS data showed the company had received $28.5 million from Nebraska Medicaid in 2024 alone, representing 33% of the state’s total ABA expenditure from a single provider. When Above and Beyond announced in late September 2025 that it was exiting the Nebraska Medicaid market entirely, the announcement sent families scrambling. One week later, the company reversed course.
THIRTY-ONE DAYS’ NOTICE AND A LEGISLATIVE BACKLASH

The compressed implementation timeline became the focal point of provider and legislative objection. When DHHS issued the July 1 notice of August 1 rate changes, providers had 31 days to respond. Some had contracts with managed care organizations that needed renegotiation; some had staffing structures that could not be sustained under the new rates; some were still waiting for formal guidance on exactly what the new rates would be for every service code. Jay Lax, founder of Silver Swing ABA in Omaha, said the pace felt calculated to prevent organized resistance rather than to enable an orderly transition.
Corey Cohrs, CEO of Radical Minds, which operates seven ABA centers in Omaha, took a different position publicly: he supported the cuts. His argument was that Nebraska’s rates had been so far above national benchmarks that the program had become a magnet for providers with questionable quality, and that a correction was overdue. His public endorsement of DHHS’s position was notable in a field where providers almost uniformly opposed the reductions.
On September 5, 2025, the Legislature’s Health and Human Services Committee convened a hearing to take testimony on the cuts. The hearing was chaired by Sen. Brian Hardin of Gering, who had called the session as part of a legislative study authorized by Legislative Resolution 191. Invited testifiers included Mariel Fernandez of CASP, Addie Angelov of the Paramount Health Data Project, and Amy Nordness of the Munroe-Meyer Institute at UNMC. Fernandez presented preliminary survey data showing that at least 135 Nebraska children had already experienced interrupted ABA services in the weeks following the August 1 cuts.
“Currently, standalone ABA therapy providers are the only entity that does not have a checks and balances in place. Vetting these organizations that serve them should be a top priority.”
— Addie Angelov, Paramount Health Data Project, September 5, 2025 legislative hearing
Angelov’s testimony at the hearing went beyond the rate cut itself. She documented that Nebraska’s ABA credentialing and billing oversight had significant gaps — a finding that would soon be amplified by the state auditor. She pointed to Indiana’s governor establishing a working group to address similar cost pressures while maintaining care, and encouraged Nebraska’s HHS Committee to consider holding all ABA providers to national standards of best practices, evaluation, and auditing. Pediatricians, insurance companies, and schools met accreditation standards, she noted. ABA providers in Nebraska did not.
THE AUDITOR’S REPORT: CREDENTIALING FAILURES AND BILLING IRREGULARITIES
On September 23, 2025, the Nebraska auditor’s team released findings from its probe of the state’s ABA service expenses. The report documented credentialing deficiencies and billing irregularities that, in the auditors’ assessment, contributed to the program’s cost escalation. The audit did not exonerate DHHS’s rate-setting process, but it did validate a core part of the state’s argument: that Nebraska’s ABA program had grown without the oversight infrastructure necessary to ensure the integrity of every dollar spent.
The specific deficiencies documented echoed what the HHS-OIG had found in Indiana the prior December: providers billing at higher individual therapy rates for what should have been group sessions; session notes that were insufficient to verify the services billed; enrolled providers who did not meet the credentialing standards the state nominally required; and claims submitted by behavioral health practitioners who had not been individually enrolled with the state’s Medicaid system. Prior to August 2025, only BCBAs had been required to individually enroll in the Heritage Health program; registered behavior technicians were not. That gap meant the state had limited ability to verify who was actually delivering services on any given claim.
DHHS’s response to the audit findings pointed to guardrails it had already begun implementing: a January 2025 directive clarifying documentation and credentialing standards; the rate reduction itself as a mechanism to reduce the financial incentive to bill questionable hours; and the August 2025 RBT enrollment requirement, which for the first time required individual registration of technicians with the Medicaid program. DHHS CEO Corsi acknowledged the program had grown faster than oversight capacity, but maintained that the rate cuts and new standards together constituted a proportionate response.
ABOVE AND BEYOND: A NEAR-EXIT THAT REVERSED IN A WEEK
The most dramatic episode of Nebraska’s rate-cut fallout came in late September 2025, when Above and Beyond Therapy — the single largest private ABA provider in the state by Medicaid billing — announced it would exit the Nebraska Medicaid market. The announcement came roughly seven weeks after the August 1 rate cuts took effect. Above and Beyond had received $28.5 million from Nebraska Medicaid in 2024 — a figure that represented both its dominant position in the market and its acute exposure to the new rate schedule. Under the post-August rates, the company said it could not sustain the care model it had built.
The reaction from families and providers was immediate. Families currently enrolled with Above and Beyond faced the prospect of losing their provider with little time to find alternatives in a state where provider capacity was already under pressure from the rate cuts. Provider organizations issued statements. Legislators who had already called a hearing renewed calls for DHHS to reconsider the pace and magnitude of its approach.
One week after the exit announcement, Above and Beyond reversed its decision and said it would remain in the Nebraska Medicaid market. The company did not detail what had changed in its assessment or whether any commitments from DHHS had been made in the interim. The reversal stabilized the immediate access situation but did not resolve the underlying tension: providers operating under rates they considered unsustainable, with a state government that had signaled its intention to hold the line.
“Nebraska had the highest reimbursement rates of any state ABA program. Even with the adjustments, commonly billed ABA rates remain higher than the national average and median.”
— Steve Corsi, CEO, Nebraska DHHS, July 2025
WHAT NEBRASKA’S CUTS MEAN FOR THE REST OF THE COUNTRY
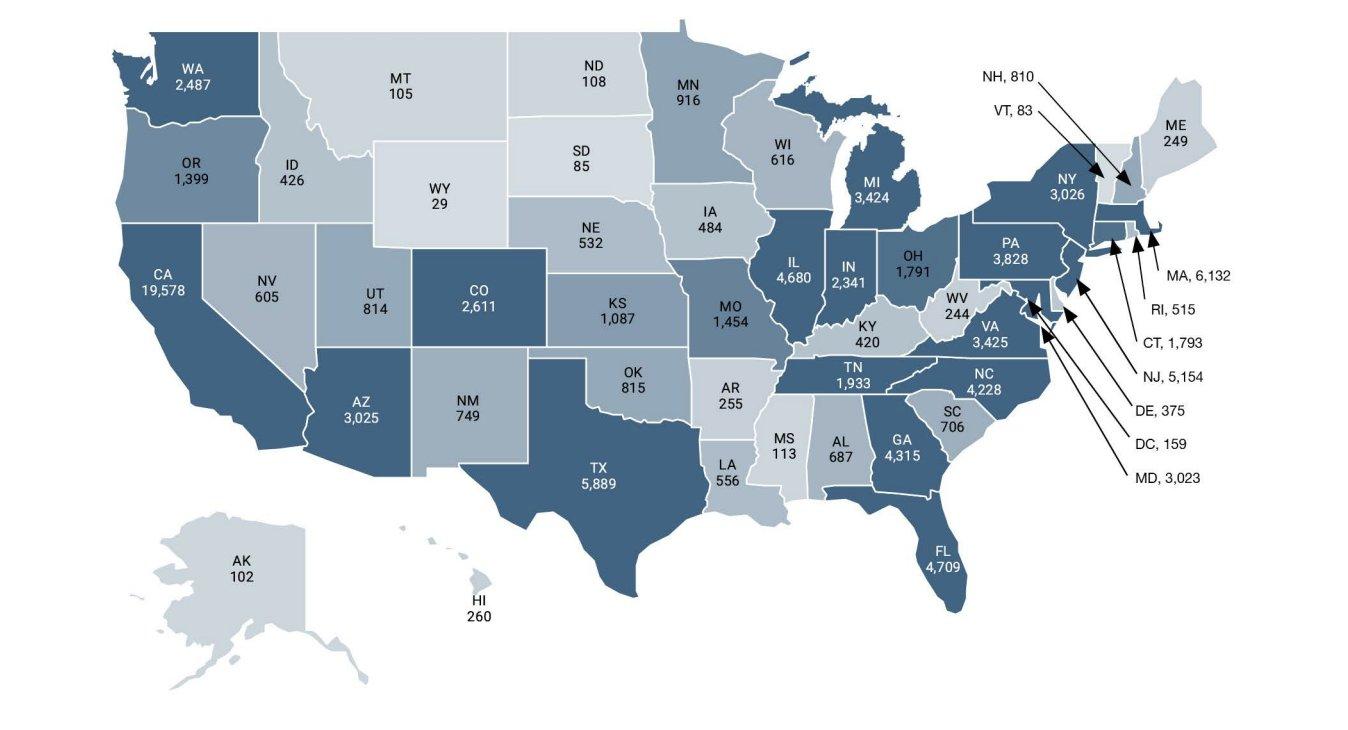
Nebraska’s August 2025 rate cuts put the state at the center of a national policy debate that is accelerating. The HHS-OIG identified ABA as a high-risk area for improper Medicaid payments and launched a nine-state audit series; Indiana was first, Wisconsin was second, and the remainder are expected to follow. North Carolina attempted a 10% ABA rate reduction effective October 2025; families of 21 children immediately sued, and the cuts were reversed in December 2025. Colorado has explored similar measures. Arizona’s managed care organizations cut provider contracts in late 2025, triggering two lawsuits and a capitol rally.
What distinguishes Nebraska’s situation is the magnitude of the cuts — up to 79% for some services, 48% for the dominant billing code — and the compressed timeline. Indiana’s working group spent months consulting providers and families before making recommendations. Nebraska gave 31 days’ notice and let the cuts take effect while the legislative hearing was still being organized. Mariel Fernandez of CASP, who testified in Lincoln, had made essentially the same point in Indiana’s working group process: the goal of sustainable rates is legitimate, but the method matters enormously for families who have no other options and for providers that cannot restructure in a month.
The audit findings that emerged in September gave Nebraska’s rate cuts a partial retrospective justification they lacked when implemented. Credentialing failures, billing irregularities, and lack of accreditation standards are real problems in Nebraska’s ABA market — problems that exist in other states too. But as Addie Angelov observed before the legislative committee, cutting rates without simultaneously building quality and accountability infrastructure is not a reform. It is a cost reduction. Whether Nebraska uses the breathing room created by lower rates to build the oversight architecture the program needs remains, as of this writing, the open question.[divider line_type=”Full Width Line” line_thickness=”1″ divider_color=”default”]Key Facts at a Glance
ABA Medicaid spending 2020: $4.6M (169 families served)
ABA Medicaid spending 2021: $10.8M
ABA Medicaid spending 2022: $23.1M
ABA Medicaid spending 2023: $51.6M (~1,150 families served)
ABA Medicaid spending 2024: $85.6M (~1,500 families served)
Growth 2020–2024: +1,750%
Rate cuts effective: August 1, 2025
Notice period: 31 days (July 1 announcement → Aug. 1 effective)
RBT therapy (97153): $36.11/unit → $18.70/unit (−48%)
BCBA supervision (97155): −37%
Parent training (97156): −51%
Treatment assessment: −28%
Group/other services: Up to −79%
Largest provider: Above and Beyond Therapy — $28.5M from Nebraska Medicaid in 2024 (33% of total)
Above & Beyond timeline: Announced Medicaid exit in late September 2025; reversed one week later
Services disrupted: At least 135 Nebraska children (preliminary CASP survey, Sept. 5, 2025 hearing)
BCBA workforce 2021: ~100 BCBAs
BCBA workforce 2024: 356 BCBAs/BCBA-Ds
BHP workforce 2020: 459 certified BHPs
BHP workforce 2024: 1,863 certified BHPs
Key Voices
Dr. Steve Corsi: CEO, Nebraska DHHS
Drew Gonshorowski: Director, Medicaid & Long-Term Care, Nebraska DHHS (started Dec. 9, 2024)
Matthew Ahern: Deputy Director / former Interim Medicaid Director, Nebraska DHHS
Sen. Brian Hardin: Chair, Legislature’s Health and Human Services Committee (Gering, NE)
Mariel Fernandez: VP of Government Affairs, Council of Autism Service Providers (CASP) — casproviders.org
Addie Angelov: Paramount Health Data Project — Sept. 5 hearing testifier
Amy Nordness: Munroe-Meyer Institute, UNMC — Sept. 5 hearing testifier
Cathy Martinez: President, Autism Family Network of Nebraska
Corey Cohrs: CEO, Radical Minds (7 Omaha locations) — publicly supported the cuts
Jay Lax: Founder, Silver Swing ABA (Omaha)
State Auditor Mike Foley: Released audit findings Sept. 23, 2025
Key Sources
Nebraska Examiner: nebraskaexaminer.com — Cindy Gonzalez, reporting July–September 2025
Legislative hearing: Sept. 5, 2025, HHS Committee, Room 1525, Nebraska Capitol (LR 191)
Nebraska Auditor’s Report: Released Sept. 23, 2025
Nebraska DHHS: dhhs.ne.gov — Drew Gonshorowski, Medicaid Director
CASP survey data: Preliminary findings presented Sept. 5, 2025 by Mariel Fernandez
Nebraska Life: nebraskalife.com
Paramount Health Data Project: Addie Angelov — accreditation and quality framework analysis











