The National Spending Surge
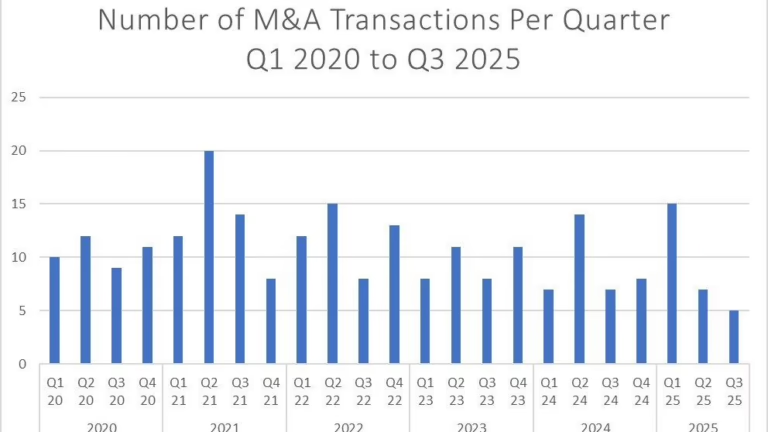
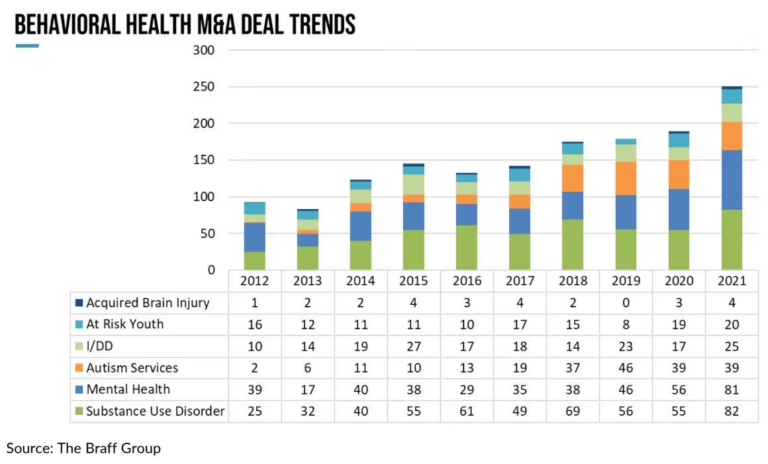
ACROSS THE UNITED STATES — state Medicaid programs are cutting ABA reimbursement after a half-decade of unchecked spending growth. Direct payments from state Medicaid programs to autism therapy providers grew to $2.2 billion in 2023 from $660 million in 2019, according to a Wall Street Journal analysis of national billing data. The number of companies offering ABA nearly doubled over the same period.
Individual state trajectories are sharper. North Carolina spending went from $122 million in fiscal 2022 to a projected $639 million in fiscal 2026, a 423 percent increase. Nebraska went from $4.6 million in 2020 to more than $85 million in 2024, roughly 1,700 percent. Indiana went from $21 million in 2017 to $611 million in 2023, a 2,810 percent increase. Minnesota’s EIDBI (Early Intensive Developmental and Behavioral Intervention) spending surged from $671,000 in 2018 to $342.8 million in 2024, more than 50,000 percent.
Four factors drove the trajectory: the 2014 CMS mandate requiring state Medicaid programs to cover autism services; rising autism diagnoses, now 1 in 31 children per the CDC; the rapid expansion of the BCBA and RBT (registered behavior technician) workforce; and the absence of cost controls in most state Medicaid programs. States built ABA benefits without rate caps, utilization limits, post-payment review, or credential verification. Spending grew accordingly.
The corrections are now underway. KFF Health News, NPR, Stateline, Governing, and Becker’s Behavioral Health have all published national analyses of the rate-cut wave. The pattern is consistent: states with the steepest spending growth are imposing the deepest cuts, often over the objections of families and providers.
It would be fiscally irresponsible of the state to maintain that. — Leila Allen, Vice President of External Affairs, Lighthouse Autism Center, on Nebraska’s rate cuts (November 2025)
State-by-State Breakdown
Nebraska. Effective August 1, 2025, Nebraska cut Medicaid reimbursement for direct ABA therapy provided by behavior technicians by 48 percent, from approximately $144 per hour to $74.80. BCBA rates dropped 37 percent. Cuts on other service codes ranged from 28 to 79 percent. The state added a 30-hour-per-week cap without additional review. Nebraska previously had the highest Medicaid reimbursement rates for ABA in the nation. Above and Beyond Therapy, paid more than $28.5 million by Nebraska’s Medicaid managed-care program in 2024, about a third of total program spending and four times the next largest provider, notified families in late September 2025 that it would terminate Medicaid participation. The company reversed course a week later, citing what it described as an outpouring of family responses. CEO Matt Rokowsky did not respond to multiple requests for comment from KFF Health News.
North Carolina. Effective October 1, 2025, North Carolina cut ABA reimbursement by 10 percent. All other Medicaid services received a 3 percent cut. The disproportionate ABA-specific cut prompted a lawsuit by the families of 21 children, filed October 31, with declarations from Compleat Kidz, Action Behavior Centers, BlueSprig Pediatrics, Already Autism Health, Centria Healthcare, and Ignited Minds. A Wake County Superior Court judge granted a preliminary injunction. In early December, Governor Josh Stein cancelled all the Medicaid cuts enacted in October, citing the lawsuits. Spending on autism services in North Carolina is projected at $639 million in fiscal 2026, up from $122 million in fiscal 2022.
Indiana. Indiana underwent the most aggressive correction. After spending peaked at $611 million in 2023, the state replaced its 40-percent-of-billed-charges reimbursement model with a flat rate of approximately $68 per hour. Spending fell to $445 million in 2024, a 27 percent reduction, without reducing the number of children served. Governor Mike Braun’s working group recommended a 4,000-hour lifetime cap, a provider moratorium, and additional reforms. FSSA Secretary Mitch Roob set an April 3, 2026 deadline for providers to self-report fraud, waste, or abusive billing practices. In March 2026, Indiana revoked the Medicaid provider agreements of Piece by Piece Autism Centers, which had received $29 million from Indiana Medicaid in 2023 to treat 84 patients, about $340,000 per child.
Colorado. Colorado is proposing rate cuts alongside expanded pre-authorization requirements. State ABA spending reached $287 million in fiscal 2025, a fivefold increase in six years. Providers and parents sued the state over the pre-authorization mandate. An HHS Office of Inspector General audit released March 2, 2026 found at least $77.8 million in improper payments and recommended a $42.6 million federal refund, plus another $112.5 million in potentially improper federal-share payments under further review. The state faces a $1 billion budget shortfall. The OIG also flagged that Colorado was paying for care delivered by 1,500 to 2,000 uncredentialed behavioral technicians.
Minnesota. Minnesota had 85 open investigations into autism providers as of summer 2025. The FBI raided two providers, Smart Therapy Center and Star Autism Center, in 2024. In December 2025, Smart Therapy owner Asha Farhan Hassan pleaded guilty to wire fraud in a $14 million autism Medicaid scheme involving unqualified staff and kickbacks of $300 to $1,500 per month to parents who enrolled their children. Hassan agreed to pay nearly $16 million in restitution. Minnesota EIDBI spending surged from $671,000 in 2018 to $342.8 million in 2024.
Washington. Washington placed limits on optional programs and home and community-based services, including ABA. The cuts disproportionately affect smaller providers, since larger chains can absorb rate reductions more easily.
Additional states where cuts have been proposed, studied, or are likely based on spending trajectories include Texas, Florida, Georgia, Arizona, and Ohio. Across the eight states with publicly available ABA data, namely Indiana, Minnesota, Colorado, Massachusetts, Nebraska, North Carolina, Wisconsin, and Maine, combined Medicaid ABA spending grew from $347 million to over $2.2 billion, a 561 percent increase, according to the American Council on Science and Health.
Provider Responses
Providers are responding through four strategies: litigation, diversification, efficiency, and exit. The North Carolina lawsuit is the litigation play: challenge the cuts in court on equal protection, due process, and Olmstead integration grounds. The preliminary injunction suggests the legal arguments have merit. Litigation is expensive and uncertain, but it produced a result.
Diversification is the strategy of adding non-ABA revenue streams: speech therapy, occupational therapy, diagnostics, school-based services. JoyBridge Kids’ acquisition of Pediatric Advanced Therapy and Cortica’s multidisciplinary model exemplify the approach. Jim Spink, CEO of Autism Care Partners, has noted that state Medicaid rate cuts are often followed by commercial payers attempting similar reductions.
Efficiency means delivering more effective treatment in fewer hours at lower cost. Catalight’s quality-over-quantity approach, AnswersNow’s all-BCBA telehealth model, and the broader dosage-reform movement all sit in this category. Providers who can demonstrate outcomes at lower intensity will be better positioned to sustain operations under reduced rates than providers whose models depend on 40-hour-per-week billing.
Exit is the last resort. Above and Beyond Therapy threatened to leave Nebraska Medicaid before reversing. Autism Learning Partners, backed by FFL Partners, announced in December 2025 that it would end ABA services in Texas effective March 21, 2026, citing rates and authorization process issues. Providers that left California and Colorado in 2022 and 2023 created access gaps that remaining operators are still filling. Exit reduces access for the most vulnerable children, those on Medicaid who cannot switch to commercial insurance, and creates the political pressure that sometimes reverses the cuts.
We’ve seen state Medicaid authorities reduce their rates, and then commercial payers try to follow suit, despite the increasing pressure on access. — Jim Spink, CEO, Autism Care Partners (November 2025)
What Comes Next
The rate-cut wave is a correction, not a crisis. States built ABA benefits without cost controls, providers built business models on unsustainable rates, and spending grew until it became politically and fiscally untenable. The correction will be painful for providers whose margins depended on the old rates. It will produce a more sustainable ABA market only if the cuts are paired with the compliance infrastructure, outcomes measurement, and utilization review that the industry has lacked.
Without those accompaniments, the cuts will simply reduce access without improving quality. North Carolina’s next legislative funding decision is expected before the state’s Medicaid program runs short of funds, projected as early as April 2026 absent action. Indiana’s self-reporting deadline lands April 3. The Colorado refund question and Minnesota’s open investigations will run through 2026. Whether commercial payers follow Medicaid’s lead, as Spink predicted, will define the second wave.
AT A GLANCE
| National ABA Medicaid (2019-2023): | $660M to $2.2B; 233% increase (WSJ) |
| Eight-state combined growth: | $347M to $2.2B; 561% increase (ACSH) |
| Nebraska: | $4.6M (2020) to $85M+ (2024); 48% RBT cut, 37% BCBA cut, effective Aug 1, 2025 |
| North Carolina: | $122M (FY22) to $639M projected (FY26); 10% ABA cut Oct 1, 2025; cancelled Dec 2025 |
| Indiana: | $21M (2017) to $611M (2023) to $445M (2024); flat $68/hr; 4,000-hr lifetime cap |
| Colorado: | $287M (FY25); $77.8M improper, $42.6M federal refund; $1B budget shortfall |
| Minnesota: | $671K (2018) to $342.8M (2024); 85 open investigations; $14M criminal case |
| Washington: | Limits on optional programs and HCBS waiver including ABA |
| Provider responses: | Litigation (NC, CO), diversification, efficiency, exit (TX, NE) |
| Key risk: | Commercial payers tracking Medicaid cuts (Spink, Autism Care Partners) |
| Next deadline: | Indiana FSSA self-reporting due April 3, 2026 |
SOURCES & REFERENCES
| 1. | KFF Health News / NPR. “It’s the ‘Gold Standard’ in Autism Care. Why Are States Reining It In?” December 23, 2025. https://kffhealthnews.org/news/article/aba-therapy-applied-behavior-analysis-autism-medicaid-rate-cuts-north-carolina/ |
| 2. | Stateline. “Families Worry as Cost of Autism Therapy Comes Under State Scrutiny.” November 25, 2025. https://stateline.org/2025/11/25/families-worry-as-cost-of-autism-therapy-comes-under-state-scrutiny/ |
| 3. | Becker’s Behavioral Health. “States Move to Cut ABA Therapy Payments as Medicaid Spending Spikes.” March 17, 2026. https://www.beckersbehavioralhealth.com/behavioral-health-government-policies/states-move-to-cut-aba-therapy-payments-as-medicaid-spending-spikes/ |
| 4. | Behavioral Health Business. “Autism Therapy Providers Fight Medicaid Rate Cuts in Court.” November 13, 2025. https://bhbusiness.com/2025/11/13/autism-therapy-providers-fight-medicaid-rate-cuts-in-court/ |
| 5. | Behavioral Health Business. “How Providers Can Future Proof Themselves as State Medicaid Agencies Cut ABA Rates.” November 13, 2025. https://bhbusiness.com/2025/11/13/how-providers-can-future-proof-themselves-as-state-medicaid-agencies-cut-aba-rates/ |
| 6. | Wall Street Journal. “The Boom in Autism Therapy Is Medicaid’s Fastest-Growing Jackpot.” March 10, 2026. https://www.wsj.com/health/healthcare/autism-therapy-medicaid-spending-aba-7b6cd45c |
| 7. | Indiana Capital Chronicle. “State coming down on autism therapy providers that potentially abused system.” March 24, 2026. https://indianacapitalchronicle.com/2026/03/24/state-coming-down-on-aba-providers-that-potentially-abused-system/ |
| 8. | American Council on Science and Health. “The Autism Therapy Gold Rush.” April 9, 2026. https://www.acsh.org/news/2026/04/09/autism-therapy-gold-rush-50049 |
| 9. | HHS Office of Inspector General. “Colorado Made at Least $77.8 Million in Improper Fee-for-Service Medicaid Payments for Applied Behavior Analysis Provided to Children.” March 2, 2026. https://oig.hhs.gov/reports/all/2026/colorado-made-at-least-778-million-in-improper-fee-for-service-medicaid-payments-for-applied-behavior-analysis-provided-to-children/ |
| 10. | Colorado Sun. “Colorado wrongly spent $78M on autism therapy, Office of the Inspector General says.” March 3, 2026. https://coloradosun.com/2026/03/02/colorado-wrongly-spent-78m-on-autism-therapy-office-of-the-inspector-general-says/ |
| 11. | Behavioral Health Business. “Autism Learning Partners to Leave Texas Market.” December 3, 2025. https://bhbusiness.com/2025/12/03/autism-learning-partners-to-leave-texas-market/ |
| 12. | Governing / KFF Health News. “States Move to Rein In ‘Gold Standard’ Autism Therapy as Medicaid Spending Surges.” January 5, 2026. https://www.governing.com/policy/states-move-to-rein-in-gold-standard-autism-therapy-as-medicaid-spending-surges |