The Paradox: High Demand, Low Supply
ATLANTA, GEORGIA – Georgia is the eighth most populous state in the country, with approximately 11 million residents. It is also, by the Behavior Analyst Certification Board’s own data, one of the five highest-demand states for BCBAs in the nation. In 2023, the BACB’s employment demand report identified California, Massachusetts, Texas, Florida, and Georgia as the five states accounting for 40 percent of all national BCBA job postings. Georgia has remained in that top tier through 2025, with the BACB’s latest report recording 132,307 total BCBA and BCBA-D job postings nationally — and Georgia continuing to absorb a significant share.
Yet the workforce available to meet that demand remains drastically undersized. Nationally, as of mid-2025, there were approximately 48,352 BCBA certificants against more than 132,000 job postings — a gap of roughly 50,000. In Georgia, the Bureau of Labor Statistics projects 21.7 percent job growth for behavior analysts from 2022 to 2032, with approximately 720 openings per year. The statewide median salary for behavior analysts in Georgia is $55,320, with the Atlanta metro area averaging $58,990 — figures that, while competitive regionally, sit well below the national average of approximately $72,450 and far below what coastal states offer.
The result is a state where demand formally exists, insurance coverage formally exists, and Medicaid coverage formally exists — but where the actual delivery of ABA services is concentrated overwhelmingly in the Atlanta metropolitan area and a handful of secondary cities, leaving the majority of the state’s geography functionally unserved.
Georgia ranks among the top five states nationally for BCBA demand, yet its rural geography, wage structure, and late-arriving licensure framework have produced one of the most acute ABA care deserts in the Southeast.
The Coverage Architecture: Three Layers, Each with Gaps
Georgia’s ABA funding landscape is built on three pillars, each of which carries structural limitations that compound the workforce shortage.
Ava’s Law (Private Insurance): Georgia’s autism insurance mandate, House Bill 429 — known as Ava’s Law — was enacted in 2015. As originally passed, it required state-regulated private insurance plans to cover ABA therapy for children. Senate Bill 118, signed in 2019, expanded coverage to individuals under age 21 and raised the annual ABA therapy cap to $35,000. The law applies to fully insured group and individual plans regulated by the Georgia Department of Insurance. It does not apply to self-funded employer plans governed by ERISA — a significant gap, since a substantial share of commercially insured Georgians are covered under self-funded arrangements. The $35,000 annual cap, while an improvement over the original law, is a hard ceiling. For a child requiring 25 to 40 hours of ABA therapy per week, annual costs can exceed $50,000 to $100,000 depending on the intensity and provider rates. The cap means that families frequently exhaust their annual benefit mid-year, creating gaps in care continuity.
Georgia Medicaid (ASD Coverage Since 2018): The Georgia Department of Community Health began providing Medicaid coverage for autism spectrum disorder services on January 1, 2018, for individuals under age 21. Coverage is administered through Care Management Organizations and is contingent on a documented DSM-V diagnosis and medical necessity determination. Georgia Medicaid covers up to 40 hours per week of ABA therapy for children under 6 and up to 25 hours per week for older children. A CSG South comparative analysis found that Georgia’s Medicaid reimbursement rates for ABA services are higher than those of most neighboring states in the region, and that Georgia uniquely designates different rates based on whether services are delivered in-home or in-clinic, with in-home rates set higher — likely to account for provider travel costs.
The Medicaid Gap: Georgia is one of only 10 states that have not fully expanded Medicaid under the Affordable Care Act. Instead, the state operates Georgia Pathways to Coverage, a partial expansion with work requirements that has enrolled only approximately 7,463 individuals as of May 2025 — against an estimated 359,000 who would be eligible under full ACA expansion. The program has spent $80.3 million since fiscal year 2021, of which $54.2 million went to administrative costs and only $26.1 million to actual health care benefits. KFF estimates that 175,000 Georgians remain in the Medicaid coverage gap: their incomes are below the poverty level, so they do not qualify for marketplace subsidies, yet they are also ineligible for Medicaid. Georgia’s overall uninsured rate of approximately 13.7 percent is the third highest in the nation. In rural counties, that figure can exceed 20 percent.
Georgia Pathways has enrolled roughly 7,463 people against an estimated 359,000 who would be eligible under full Medicaid expansion. The state has spent $80.3 million on the program — 67 percent of which went to administrative costs.
The Rural Reality: 159 Counties, Most Without a BCBA
Georgia’s geography is the single most defining feature of its ABA access crisis. The state has 159 counties — second only to Texas among U.S. states. At least 118 of those counties are classified as rural, with populations below 50,000. National research indicates that only about 12 percent of behavior analysts practice in rural areas, and as of July 2018, approximately 54 percent of all U.S. counties had no BCBAs at all. While that figure has improved to roughly 46 percent nationally, Georgia’s county structure — with its unusually high number of small, low-population jurisdictions — means that a disproportionate share of its territory falls into the zero-BCBA category.
For families in rural southwest Georgia, the Piedmont, or the coastal plain south of Savannah, the nearest ABA provider may be hours away. Children with ASD in these areas who are recommended for 20 to 40 hours of weekly therapy face a logistical impossibility: the travel burden alone can consume a double-digit number of hours per week. Research on rural ABA access has documented that children with ASD living in rural versus urban areas are significantly more likely to report difficulties and delays due to lack of available services — 35 percent in rural areas compared to 23 percent in urban areas, a 12-percentage-point gap that represents thousands of children missing critical developmental intervention windows.
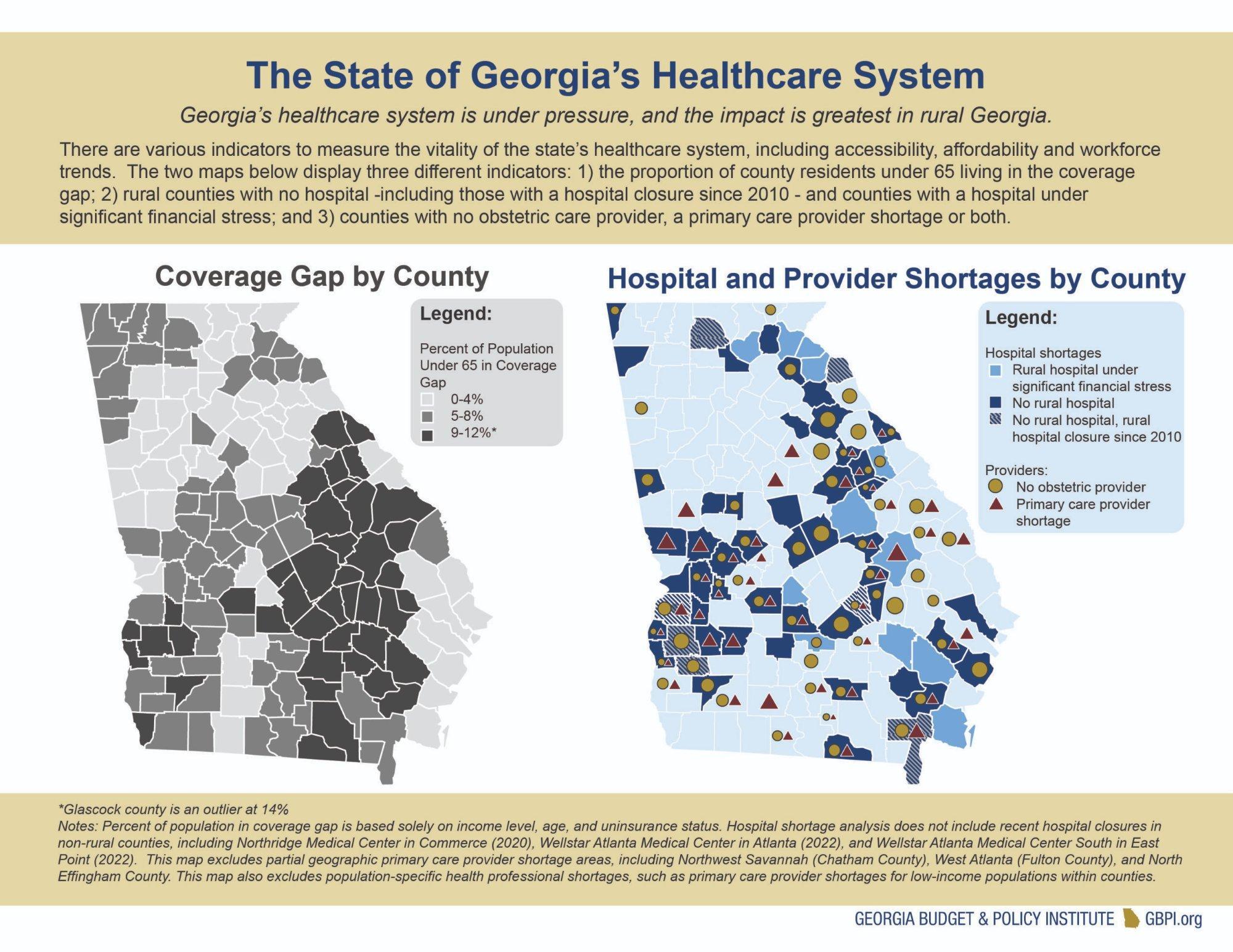
The problem is compounded by the state’s rural hospital crisis. At least seven rural hospitals in Georgia have closed since 2013, and more than half of the state’s remaining rural hospitals are classified as financially vulnerable to closure. These closures eliminate not only emergency and primary care infrastructure but also the referral pathways through which developmental concerns are identified and children are connected to diagnostic evaluation and ABA services. When the nearest hospital closes, the nearest developmental pediatrician moves further away — and the already-long pipeline from symptom recognition to ASD diagnosis to ABA referral grows longer.
Licensure: A Late-Arriving Framework
Georgia’s behavior analyst licensing infrastructure is newly operational. The Georgia Behavior Analyst Licensing Board began accepting applications in 2025, with practicing behavior analysts required to submit complete licensure applications by September 30, 2025, and assistant behavior analysts by March 31, 2026. The Board uses BCBA and BCaBA certification as the basis for state licensure.
The significance of this timing is that Georgia operated for years without a state licensing requirement for behavior analysts, meaning that the regulatory infrastructure that supports workforce development, consumer protection, and payer credentialing was absent during the period of greatest ABA demand growth. States that established behavior analyst licensing earlier — such as Massachusetts, which has been among the first movers in both licensure and insurance mandates — have generally built larger, more stable BCBA workforces relative to demand. Georgia’s late start means the state is building licensure infrastructure at the same time it is trying to close a workforce gap that has been widening for over a decade.
The Budget Picture: Incremental Investment in a Structural Problem
Georgia’s fiscal year 2026 budget, administered through the Department of Community Health, includes approximately $23 million in additional state funds for Medicaid provider rate increases. The largest rate increase categories include emergency medical transportation, therapy for children with autism, newborn deliveries in rural counties, and primary care. The autism-specific rate increase is a positive signal, but the overall scale of the investment is modest relative to the structural deficit in ABA access.
Total state funding for the Department of Community Health in FY 2026 is approximately $5.6 billion, with about 94 percent earmarked for Medicaid and PeachCare. The federal government provides approximately $14 billion in combined support across Georgia’s three primary health agencies. The state’s decision not to fully expand Medicaid means it foregoes approximately $3 billion per year in federal health care funding that would otherwise flow into Georgia — money that, in states like North Carolina which adopted expansion more recently, has been used to dramatically expand coverage. North Carolina enrolled 553,890 people in its first period of Medicaid expansion, with 37 percent of enrollees living in rural counties.
For ABA providers, the fiscal environment in Georgia presents a mixed picture: Medicaid reimbursement rates are regionally competitive, but the population of Medicaid-eligible individuals who can access services is constrained by the coverage gap. The $35,000 annual cap on private insurance ABA benefits limits revenue per patient. And the rural geography means that any provider willing to serve outside the Atlanta metro must contend with high travel costs, low population density, and a workforce that overwhelmingly prefers urban practice settings.
What Would Close the Gap
The Georgia ABA access problem is not a single-variable failure. It is a system in which workforce shortage, insurance limitations, Medicaid contraction, geographic reality, and late licensure infrastructure all reinforce one another. Addressing it would require simultaneous action across multiple dimensions.
Full Medicaid expansion: Closing the coverage gap would bring an estimated 359,000 Georgians into Medicaid eligibility, generating a new patient population for ABA providers and creating the economic conditions — through additional federal funding — to stabilize rural health infrastructure.
Elimination or significant increase of the $35,000 annual ABA cap: The current Ava’s Law ceiling runs out mid-year for many families with children in intensive ABA programs. Raising or removing the cap would align Georgia with states that have uncapped ABA mandates.
Rural workforce incentives: Loan repayment programs, rural practice bonuses, or tax incentives for BCBAs who practice outside the Atlanta metro could begin to shift the geographic distribution of the workforce. Models from other health professions — including the National Health Service Corps — provide templates.
Telehealth infrastructure investment: Telehealth-delivered ABA supervision and parent training can extend BCBA reach into areas where in-person service delivery is logistically impractical. However, broadband access remains a barrier: nationally, 28 percent of rural residents lack access to high-speed internet, and Georgia’s rural broadband gaps mirror this pattern.
University pipeline expansion: Georgia’s BCBA training capacity must expand to match projected demand of 720 openings per year. Partnerships between regional universities and ABA provider organizations — offering tuition support in exchange for rural practice commitments — could accelerate pipeline development.
Georgia has the demand, the legal framework, and the clinical need. What it lacks is the operational infrastructure to convert those conditions into access. Until the state addresses the structural barriers — the Medicaid gap, the insurance cap, the rural geography, and the workforce pipeline — it will remain one of the most populous ABA deserts in the country.
AT A GLANCE
Georgia population: Approximately 11 million (8th most populous U.S. state)
Counties: 159 — second only to Texas. At least 118 classified as rural (population below 50,000).
BCBA demand ranking: Top 5 nationally (CA, MA, TX, FL, GA account for 40% of all BCBA job postings, BACB/Lightcast 2023)
Projected BCBA job growth: 21.7% from 2022–2032, with ~720 openings per year (BLS)
BCBA median salary (GA): $55,320 statewide; $58,990 in Atlanta metro (BLS)
Ava’s Law (HB 429/SB 118): Private insurance must cover ABA up to $35,000/year for individuals under 21
Medicaid ABA coverage: Since January 1, 2018. Up to 40 hrs/week (under 6) or 25 hrs/week (6+). Medical necessity required.
Medicaid expansion status: Not fully expanded. Georgia Pathways enrolled ~7,463 as of May 2025 vs. 359,000 estimated eligible.
Uninsured rate: ~13.7% (3rd highest nationally). Rural counties may exceed 20%.
Rural hospital closures: At least 7 since 2013; more than half of remaining rural hospitals financially vulnerable.
Behavior analyst licensure: Georgia Licensing Board operational 2025. BCBA applications due September 30, 2025.
Rural ABA access gap: 35% of rural ASD families report service difficulties vs. 23% in urban areas (12-point gap).
SOURCES & REFERENCES
1. – BACB & Lightcast. US Employment Demand for Behavior Analysts: 2010–2025. February 2026. Reported by Behavioral Health Business. https://bhbusiness.com/2026/02/17/demand-for-bcbas-continues-exponential-growth-despite-slight-slowdown/
2. – Behavioral Health Business. “Demand for BCBAs Vastly Outstrips the Total Workforce.” March 2024. https://bhbusiness.com/2024/03/25/demand-for-bcbas-vastly-outstrips-the-total-workforce/
3. – Applied Behavior Analysis EDU. How to Become a BCBA in Georgia. 2025. https://www.appliedbehavioranalysisedu.org/georgia/
4. – Georgia Department of Community Health / Georgia Medicaid. Autism Spectrum Disorder Coverage. 2018. https://medicaid.georgia.gov/programs/all-programs/autism-spectrum-disorder
5. – Georgia Legislature. House Bill 429 (Ava’s Law), 2015; Senate Bill 118, 2019. Georgia Code § 33-24-59.10.
6. – Council of State Governments South. Comparison of Medicaid Reimbursement for ABA Individual Services. 2024. https://csgsouth.org/wp-content/uploads/HSPS-Converted-IR__Comparison-of-Medicaid-Reimbursement-for-ABA-Individual-Services.pdf
7. – Georgia Budget and Policy Institute. Fast Facts on Medicaid Expansion. 2020 (updated). https://gbpi.org/fast-facts-on-medicaid-expansion/
8. – Georgia Budget and Policy Institute. Georgia Health Primer for State Fiscal Year 2026. July 2025. https://gbpi.org/georgia-health-primer-for-state-fiscal-year-2026/
9. – Georgia Recorder. “Georgia’s limited Medicaid expansion program is extended through 2026.” September 2025. https://georgiarecorder.com/2025/09/26/georgias-limited-medicaid-expansion-program-is-extended-through-2026-despite-concerns-about-cost/
10. – Georgetown University CCF. “Georgia’s Pathways to Coverage Has Turned Into Pathways to Profit.” October 2024. https://ccf.georgetown.edu/2024/10/30/georgias-much-vaunted-medicaid-waiver-pathways-to-coverage/
11. – KFF. Status of State Medicaid Expansion Decisions. 2025. https://www.kff.org/medicaid/status-of-state-medicaid-expansion-decisions/
12. – HealthInsurance.org. Medicaid Eligibility and Enrollment in Georgia. 2025. https://www.healthinsurance.org/medicaid/georgia/
13. – TYGES Healthcare. Applied Behavioral Analysis Care Deserts in the U.S. February 2026. https://tyges.com/healthcare-practice/behavioral-health-care-deserts/
14. – Links ABA. ABA in Underserved Communities: Bridging the Gap. August 2025. https://linksaba.com/aba-in-underserved-communities-bridging-the-gap/
15. – Apex ABA. Challenges of ABA Therapy for Autism in Rural Georgia. 2025. https://www.apexaba.com/blog/challenges-of-aba-therapy-for-autism-in-rural-georgia
16. – WeAchieve ABA. BCBA Job Growth 2025. 2025. https://www.weachieveaba.com/blogs/bcba-job-growth-2025-why-demand-is-outpacing-available-professionals
17. – ABA Centers of Georgia. A Helpful Overview of ABA Insurance Coverage in Georgia. May 2025. https://www.abacentersga.com/blog/aba-insurance-coverage/
18. – Cover Georgia. Medicaid Expansion FAQs. 2024. https://coverga.org/medicaid-expansion/faqs/











