PHOENIX, AZ — On the morning of March 5, 2026, Kim Powell carried her four-year-old son Teddy to a microphone outside the Arizona State Capitol and let him speak for himself. He spelled his name — T-E-D-D-Y — clearly and without hesitation, then announced: “My name is Teddy.” A year earlier, he had been nonverbal. That progress, his mother told the crowd, was entirely the product of applied behavior analysis therapy at the provider Mercy Care had just dropped from its network.
As of that week, Teddy’s insurer no longer covered the clinic where he’d made that progress. The other options listed as in-network, his mother said, were not logistically reachable for her family. The story Powell told in front of the capitol — a child who gained a voice, then risked losing the care that gave it to him — was one of nearly 1,000 similar stories playing out simultaneously across Arizona, the direct consequence of a billing dispute between a Medicaid insurer and two ABA providers that AHCCCS, the state’s Medicaid agency, approved without independently verifying that families would actually be able to access alternatives.
“This is not a luxury. This is the difference between a child thriving and disappearing back into silence.”
— Elizabeth Galvez, mother of three boys with autism, two of whom were nonverbal before ABA
How a rate dispute became an access crisis
The sequence of events that produced the March 2026 crisis began in July 2025, when Mercy Care — a nonprofit Medicaid insurer operating under contract with AHCCCS — cut its reimbursement rates for ABA therapy across its network by 15%. Centria Autism, one of the largest ABA providers in the state with roughly 260 Arizona clients on Medicaid, absorbed the reduction. Then, on September 19, 2025, Mercy Care notified Centria of a second proposed cut: another 25%, effective October 1.
Centria’s legal team sent a letter to AHCCCS the same month, laying out the math. Combined, the two cuts would amount to a 40% reduction in the rates Mercy Care paid for ABA services in under twelve months. Centria’s position was that operating under those terms would require a fundamental restructuring of its care model, making it impossible to continue delivering the level of services its clients required. The company submitted counterproposals, including a smaller cut and a performance-based pay component. Mercy Care did not respond to those proposals. On October 17, it sent a contract termination notice.
The contract termination date moved several times, eventually settling on March 5, 2026 — the same day families rallied at the capitol. Action Behavior Centers (ABC), the other major provider caught in the restructuring, faced parallel terminations from Mercy Care, Arizona Complete Health, and UnitedHealthcare Community Plan. Together, Centria and ABC operated approximately 50 ABA facilities statewide. Their removal from the network did not affect whether ABA was a covered benefit under AHCCCS — it remained one — but it immediately narrowed which providers could deliver that benefit to Medicaid enrollees.
TIMELINE: FROM RATE CUT TO CAPITOL RALLY
Jul 2025 — Mercy Care cuts ABA reimbursement rates 15% across its network.
Sep 19, 2025 — Mercy Care proposes additional 25% rate cut to Centria, effective Oct. 1.
Oct 17, 2025 — Mercy Care sends contract termination notice to Centria after counterproposals go unanswered.
Nov 2025 — AHCCCS tells affected families it cannot intervene in MCO contract decisions.
Dec 9, 2025 — Mercy Care notifies Centria it will not continue negotiations; termination final.
Dec 15, 2025 — LAWSUIT 1: Centria + two families sue Mercy Care, AHCCCS, and Arizona DES.
Late 2025 — ~1,000 Arizona families notified that Centria and ABC will be dropped from network in March 2026.
Feb 6, 2026 — LAWSUIT 2: Class-action filed by 11 families against AHCCCS, Mercy Care, and Arizona Complete Health.
Mar 5, 2026 — Contract terminations take effect. Families rally at Arizona State Capitol. Court injunction decision expected within days.
The Ghost Network: 70 Providers on Paper, Far Fewer in Practice
Mercy Care’s public position throughout the dispute was consistent: its network of more than 70 in-network ABA providers across Arizona was sufficient to absorb the families losing coverage through Centria and ABC. In a declaration filed with the court, Mercy Care laid out a time-and-distance analysis showing that, with the exception of families in rural areas, each affected member had at least one alternative provider with capacity in their geographic area. “We are confident that our statewide network of over 70 ABA providers can ensure continuity of care for our members,” the insurer stated publicly.
Parents, providers, and attorneys representing the families described a different reality on the ground. Families who had been attempting to find alternative placements for weeks — some since receiving termination notices in November and December — reported waitlists stretching six months to a year at remaining in-network centers. Providers that appeared in the network directory, families said, had no actual openings, did not take Medicaid for new clients, or were not equipped to serve children with more intensive needs. Attorney Michael Easley Jr., representing families in the class-action suit, told the Arizona Mirror that this pattern had a name: a ghost network.
“Some managed care providers intentionally make it difficult for enrollees to access care. The more therapies provided to each client, the less money the managed care organization makes.”
— Michael Easley Jr., attorney, class-action lawsuit
The structural incentive Easley described is a defining feature of the managed care model. AHCCCS pays Mercy Care, Arizona Complete Health, and other Medicaid managed care organizations a fixed monthly capitated rate per enrolled member. The MCO keeps whatever portion of that payment is not spent on services. The less care delivered, the more an MCO retains. Expensive services — and ABA, at 40 hours per week for young children with severe autism, is among the most expensive — are precisely the category that drives the most financial pressure within that model.
The lawsuit filed on behalf of the 11 families pointed to a specific violation of those requirements. AHCCCS’s own rules, attorney Tim Nelson told the court, mandate continued provision of behavioral health services “according to the needs of the person” — but no longer than 45 days after the need is identified. Waitlists at available providers were already far exceeding that threshold before the contract terminations. “Many providers’ waitlists far exceed those limits,” Nelson said. The network that was supposed to absorb 1,000 displaced families was, by plaintiffs’ account, already at capacity before those families needed to use it.
Separately, the suits noted that AHCCCS had taken Mercy Care’s word on network adequacy without conducting an independent verification. AHCCCS, in its own court declaration, rejected this characterization: “That AHCCCS has not done some of the specific things that Plaintiffs want does not mean AHCCCS has not engaged in proper oversight of its MCOs.” The agency maintained it cannot approve or deny individual subcontractor terminations — that authority, it argued, rests with the MCOs under the terms of their contracts.
For Families, the Math Is Impossible
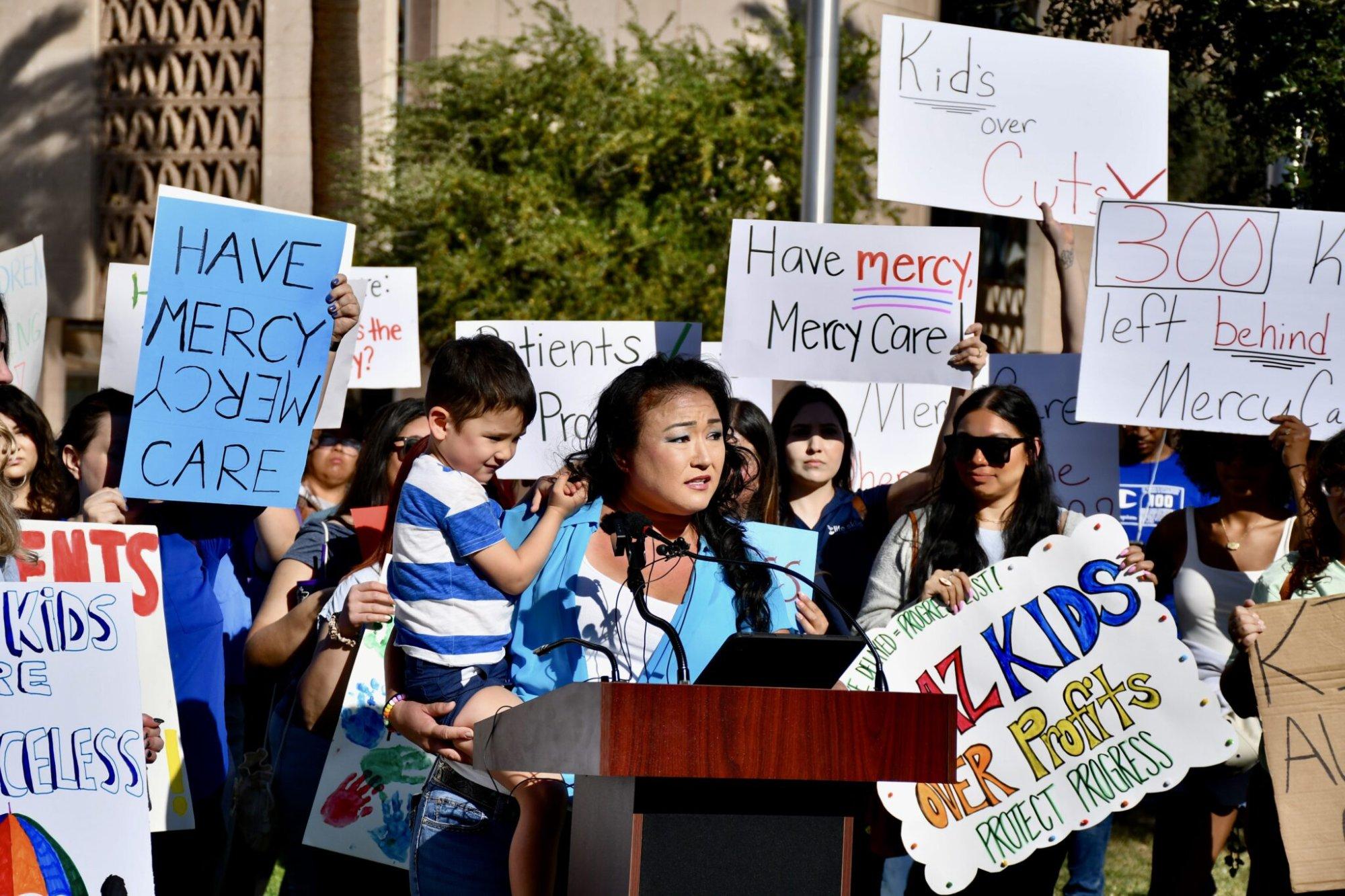
The families caught in the network disruption were not evenly distributed across the severity spectrum. Several of the children whose cases appear in the lawsuits carry Level 3 autism diagnoses — the most severe classification under DSM-5 — and are fully nonverbal. Colin, the five-year-old son of Chandler mother Melissa Fernandez, is one of them. He was diagnosed at age 2, began ABA at the same time, and has since progressed to a point where he can follow directions well enough to complete swim lessons and eat dinner with his family. “Maybe we’re not where other 5-year-olds are, but we’re getting there through ABA,” Fernandez said. Any lapse in services, she said, would mean visible regression within days.
Three-year-old Aiden, the son of single mother Lea Zibeth, had been nonverbal when he started 40-hour-per-week ABA in August 2025. He began speaking in February 2026 — his first words. Zibeth had been on a waitlist for eight months before securing that placement. After the contract terminations, Aiden received a one-time service extension through May 2026. After that, Zibeth told Axios, she will likely need to quit her job to care for him full time.
The out-of-pocket cost of continuing ABA therapy outside the Medicaid network underscores why these families have no realistic fallback. Advocate Jonna Lang told KTAR that in at least one case, an Arizona mother had canceled her own health insurance policy to free up $600 per month — the cost of continuing ABA for her son without Medicaid coverage. That figure represents a fraction of the actual market rate for intensive ABA, suggesting the family was managing a steep discount arrangement. For families without similar options, the choice is between waiting a year for a new in-network placement and watching a child regress, or finding money that does not exist.
Two Lawsuits, One Question: Who Is Accountable?
The legal strategy against AHCCCS is twofold, and the two suits approach liability differently. The first suit, filed December 15, 2025 by Centria and two families, names Mercy Care, AHCCCS, and the Arizona Department of Economic Security as defendants. It alleges the contract termination violated state and federal regulations requiring AHCCCS approval before major network changes and requiring MCOs to maintain comprehensive behavioral health networks. Mercy Care’s contract with Centria contained language permitting termination “for any reason or no reason at all” — language Centria’s attorneys argue cannot override federal Medicaid network adequacy requirements.
The second suit, the class action filed February 6, 2026 on behalf of 11 families, takes a different angle. Attorney Tim Nelson named only AHCCCS as the defendant, not the insurers. His theory of liability is that the federal Medicaid Act and its implementing regulations place the obligation to ensure adequate care access squarely on the state agency — not on the MCOs it contracts with. AHCCCS, he argued, had approved a network change without verifying the network could actually absorb the displaced families, in violation of both its own rules and federal law. The suit sought an immediate temporary restraining order to halt the terminations; a ruling was expected within days of the March 5 rally.
AHCCCS pushed back, arguing that the families’ dispute was with Mercy Care, not with the agency, and that a court order against AHCCCS would not have the practical effect of reinstating the contracts. The agency’s attorneys characterized the families’ attachments to their existing providers as “emotionally charged preferences” that did not rise to the legal threshold of irreparable injury. Attorneys for the 11 families countered that the resistance to switching was not emotional but logistical: transportation barriers, no rural providers, reduced service hours at alternatives, and the clinically documented harm that comes from disrupting therapy for children whose progress depends on consistent routine.
“Continuity of care is critical for children with autism, who often struggle to cope with even minor changes in established routines. Loss of access to ABA or forcing children to change providers is certain to cause regression and irreparable harm.”
— Attorney Tim Nelson, class-action complaint, February 2026
The Cost Pressure Beneath the Contracts

To understand why Mercy Care moved so aggressively on rates, it is necessary to understand the financial condition of Arizona’s Medicaid disability program. AHCCCS spent $371 million on ABA services in 2025, up from $260 million the prior year — a 43% increase in a single year. That growth sits inside a broader budget crisis within the Division of Developmental Disabilities (DDD), the AHCCCS program that funds ABA alongside other services for Arizonans with disabilities. Qualifying autism diagnoses in Arizona have increased by roughly 1,000% since 2006. Enrollment in DDD has surged over the past five years at a pace the agency’s budget was not structured to absorb.
The financial stress came to a head in 2025. Arizona’s legislature and Governor Katie Hobbs reached an emergency funding agreement to prevent a budget crisis at DDD, but the deal came with new guardrails designed to slow cost growth. As of the March 2026 crisis, many of those guardrails had not yet been implemented. Governor Hobbs’ FY 2026 budget proposal included a nearly $300 million increase for DDD — an acknowledgment that prior funding levels were structurally insufficient. Federal funding uncertainty compounded the picture: new Medicaid requirements signed into law by President Trump were expected to cost AHCCCS hundreds of millions in federal dollars over the following years.
Against that backdrop, Mercy Care’s rate cuts were not entirely disconnected from real fiscal pressure. The insurer characterized its decisions as responsible stewardship of Arizona taxpayer funds. What made the situation exceptional was not that an insurer tried to reduce costs — that is structurally built into the capitated Medicaid model — but the size and speed of the proposed cuts (40% in one year), the absence of any verified transition plan before the terminations were finalized, and the pre-existing shortage of ABA providers in Arizona that made the “70-plus alternative providers” claim difficult to sustain on the ground.
Matt Stringer, chief marketing officer of Action Behavior Centers, put it directly: “We are disappointed that Mercy Care unilaterally chose to terminate agreements with ABA therapy providers after proposing crippling cuts that would make it untenable to continue delivering services. Arizona already has one of the largest ABA therapy provider shortages in the country, leaving many families on long waitlists.”
Arizona Is Not Alone — but Its Mechanism Is Different
Arizona’s situation sits within the same national cost-pressure wave that triggered Nebraska’s rate cuts, Indiana’s working group, and legislative battles in North Carolina and Colorado. ABA spending has grown faster than state Medicaid budgets expected in nearly every state that expanded coverage, and managed care organizations in multiple states have begun pushing back on the rates they pay large multi-state ABA providers. But Arizona’s mechanism is distinct from states that cut rates legislatively or through direct state action.
In Indiana, the cuts were proposed by FSSA — a state agency — and subjected to public process before implementation. In Nebraska, the cuts were promulgated by the state Medicaid agency with public notice. In Arizona, the cuts were initiated by a private nonprofit insurer operating under a capitated Medicaid contract, approved by the state without independent network adequacy verification, and took effect on a timeline determined by the MCO’s internal contracting calendar. The families affected had no meaningful role in a process they were notified about only after it was already decided. That structural difference — cost pressure laundered through an MCO rather than owned by a state agency — is precisely what the lawsuits aim to address. Whether AHCCCS has a legal obligation to intervene when its contractors make network changes that result in inadequate access is the question the Arizona courts are now being asked to answer.[divider line_type=”Full Width Line” line_thickness=”1″ divider_color=”default”]KEY FACTS AT A GLANCE
Affected families: ~1,000 Arizona children on Medicaid-funded ABA
Providers dropped: Centria Autism and Action Behavior Centers (ABC)
Insurers terminating: Mercy Care, Arizona Complete Health, UnitedHealthcare Community Plan
State Medicaid agency: AHCCCS (Arizona Health Care Cost Containment System)
ABA facilities affected: ~50 Centria and ABC locations statewide
Rate cuts by Mercy Care: 15% in July 2025, then proposed 25% more in September 2025 = 40% total in under 1 year
AHCCCS ABA spending 2024: $260 million
AHCCCS ABA spending 2025: $371 million (+43% year-over-year)
AZ ABA provider shortage: Est. 22,000 AZ children with autism unable to access ABA (pre-termination)
In-network alternatives: Mercy Care claims 70+ ABA providers; families report waitlists of up to 1 year
AHCCCS insurance switch rule: Members can only switch MCOs during their child’s birth month
Out-of-pocket ABA cost: Approx. $600/month minimum for private-pay ABA (one reported case)
Centria ownership: Thomas H. Lee Partners (private equity)
THE TWO LAWSUITS
Lawsuit 1 (Dec 15, 2025): Centria Autism + 2 families vs. Mercy Care, AHCCCS, Arizona DES — Maricopa County Superior Court
Lawsuit 2 (Feb 6, 2026): Class action — 11 families vs. AHCCCS, Mercy Care, Arizona Complete Health — seeks injunction and class status
Legal theory (Lawsuit 1): Contract termination violated state/federal network adequacy rules; AHCCCS failed oversight duty
Legal theory (Lawsuit 2): AHCCCS violated federal Medicaid Act; 45-day access mandate already unmet before terminations
AHCCCS defense: Cannot approve/deny MCO subcontractor decisions; families’ dispute is with Mercy Care, not the agency
Court ruling: Expected days after March 5, 2026 rally; injunction decision pending
KEY VOICES
AHCCCS: Arizona Health Care Cost Containment System — azahcccs.gov
Mercy Care: Nonprofit Medicaid insurer — mercycareaz.org
Matt Stringer: Chief Marketing Officer, Action Behavior Centers
Tim Nelson: Attorney, class-action lawsuit (11 families)
Michael Easley Jr.: Attorney, class-action lawsuit
Jonna Lang: Family advocate, autism parent community
Elizabeth Galvez: Mother of 3 boys with autism; rally speaker
Melissa Fernandez: Chandler mother; plaintiff; son Colin, age 5, Level 3 autism
Kim Powell: Mother of Teddy, age 4; rally speaker
Renee Bradley: Mother of two children with autism; rally speaker
Lea Zibeth: Single mother; son Aiden, age 3; first words February 2026
Tiana Brandon: Gilbert mother; plaintiff; son Micah, age 6; Centria client since 2023
KEY SOURCES
Arizona Mirror: azmirror.com — Mar. 5, 2026 (Caitlin Sievers)
KJZZ: kjzz.org — ongoing coverage November 2025–March 2026
Arizona Capitol Times: azcapitoltimes.com — November 2025, February 2026
Behavioral Health Business: bhbusiness.com — “Centria Sues MCO, State Agencies” (Dec. 30, 2025)
Axios Phoenix: axios.com/local/phoenix — March 6, 2026 (Jessica Boehm)
ABC15 / AZFamily: azfamily.com — March 5, 2026
KTAR News: ktar.com — March 5–6, 2026











