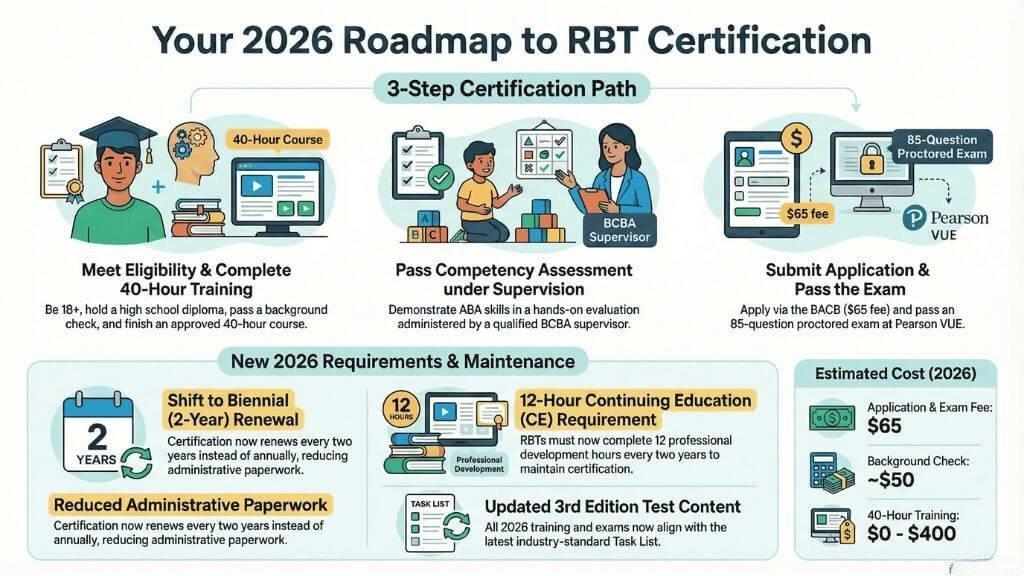
What Changed on January 1
ACROSS THE UNITED STATES — As of January 1, 2026, the Behavior Analyst Certification Board requires all new RBT applicants to complete a 40-hour training based on the third edition Test Content Outline. Applications submitted using the previous second edition curriculum are now immediately rejected. The training curriculum has been substantially updated to reflect current clinical standards and professional expectations for direct care staff. For new RBTs entering the pipeline, the bar is higher from day one.
The renewal structure has also changed. RBT certification renewals shift from an annual to a biennial (two-year) cycle, with each renewal now requiring completion of 12 hours of professional development units (PDUs) or continuing education units (CEUs). Current RBTs must complete a recertification competency assessment to transition to the new cycle. After completing the assessment, they will have two years until their next renewal and must accumulate the 12 PDUs/CEUs during that interval.
Fee increases accompany the structural changes. The initial application fee rises from $50 to $65. The renewal fee, previously $35 annually, becomes $50 biennially—a net cost reduction in dollar terms over the two-year cycle, but a change that nonetheless requires providers to adjust their administrative processes. The combined effect of new training requirements, ongoing professional development mandates, and adjusted fees represents the most significant overhaul of the RBT credential since its introduction in 2014.
The BACB’s updated standards represent the most comprehensive overhaul of the RBT credential since its creation. The question for ABA providers is not whether the changes improve quality—they almost certainly do—but whether the industry’s operational infrastructure can absorb the cost.
The Turnover Problem the Standards Walk Into
The new requirements arrive in an industry where direct care staff turnover is not a risk factor—it is a defining structural characteristic. According to the 2022 ABA Compensation and Turnover Report published by the Behavioral Health Center of Excellence, the median tenure for behavioral technicians and RBTs is one year, with an average turnover rate of 65 percent in 2021 for direct care staff. CentralReach’s Autism and IDD Care Market Report for 2025–2026 found that overall ABA industry turnover rates range from 76.7 to 90.1 percent, though this figure is not differentiated by role. Some large ABA organizations report annual turnover at or above 100 percent, driven primarily by RBT-level staff.
The drivers of this turnover are well documented. A 2025 BACB exit survey distributed to 30,018 individuals who let their RBT certification expire found that 44 percent of former RBTs reported poor treatment by their company, and 27 percent felt isolated in the workplace. Burnout from the physical and emotional demands of direct care, unstable schedules driven by last-minute client cancellations, inconsistent hours, limited career growth pathways, and compensation that often fails to keep pace with inflation all contribute to a cycle of hiring, training, and losing staff that drains provider economics.
The cost of this turnover is not abstract. Recruiting and onboarding a new RBT or BCBA can cost 30 to 200 percent of their annual salary, according to industry estimates. Lost productivity affects authorized hours and client satisfaction. Reduced continuity of care diminishes clinical outcomes and increases family churn. For ABA practice owners, the 40-hour training investment in each new hire is now more expensive in both time and direct cost—meaning that every RBT who leaves within their first year represents a larger sunk cost than before the standards changed.

The Provider Cost Calculus
The direct cost of the 40-hour training curriculum is the most visible expense, but it is not the most significant. Most large ABA providers already paid for RBT training as part of their onboarding process, and many offered the training at no cost to recruits. The shift to the third edition curriculum means providers must update their training programs, retrain their trainers, and absorb the cost of any candidates who began under the second edition but did not complete in time. For providers using external training platforms like CentralReach’s Learning Management System or ATCC’s online programs, the transition requires verifying curriculum alignment with the 2026 requirements.
The ongoing professional development requirement—12 PDUs/CEUs per two-year cycle—introduces a new recurring cost that did not exist under the previous annual renewal structure. Whether providers absorb this cost, pass it to employees, or use it as a retention incentive will vary by organization. Providers who reimburse or fund CEUs for their RBTs can use the benefit as a competitive advantage in recruitment and retention. Providers who do not risk accelerating the departure of RBTs who are unwilling to pay out of pocket for professional development in a role that already carries compensation concerns.
Emily Lorah, executive director of ABA services and regional centers at Roman Empire Agency, framed the tension directly in comments to Behavioral Health Business. She noted that ABA is not an easy service to provide and that it is positive that the BACB is increasing requirements and CEUs. But she also acknowledged that the higher bar makes the candidate pool smaller, because not everyone will want to pursue or maintain the certification under more demanding conditions. The trade-off is straightforward: clients will receive better quality service from RBTs who meet the new standards, but the supply of people willing to become and remain RBTs may contract further in a market that is already short.
The 12-hour professional development requirement is where the cost question becomes a retention question: providers who fund CEUs for their RBTs gain a competitive advantage in recruitment, while providers who shift that cost to employees risk losing staff who are already questioning whether the role is financially sustainable.
The Reimbursement Angle
Some ABA providers see the new standards as a potential lever for reimbursement negotiations. If the RBT credential now requires more training, more ongoing education, and more rigorous competency assessments, the argument for higher reimbursement rates for RBT-delivered services becomes stronger. The logic is that a more qualified workforce justifies a higher rate per billable hour—an argument that insurers have historically resisted but that the new BACB standards give providers additional evidence to support.
The reimbursement argument is particularly relevant in markets where RBT rates have not kept pace with the cost of maintaining the credential. In states with low Medicaid reimbursement rates for ABA services, the gap between what it costs to train, certify, and retain an RBT and what the payer reimburses for that RBT’s billable time has been widening. The new standards widen it further—and in doing so, may create the policy pressure needed to force rate adjustments that incremental advocacy has not achieved.
Whether payers respond to this pressure is uncertain. Commercial insurers have their own actuarial models. State Medicaid programs face budget constraints that are intensifying under the current federal administration. But the argument that a more credentialed workforce merits higher reimbursement is defensible, and the BACB’s decision to formalize the RBT’s professional development trajectory gives providers a concrete artifact to cite in rate negotiations.
The Career Pathway Question
Beyond the immediate cost and compliance dimensions, the new standards signal a shift in how the BACB conceives of the RBT role. By introducing biennial renewal, professional development requirements, and a more rigorous training curriculum, the certification board is moving the RBT credential closer to a professional certification and further from a basic entry-level qualification. This has implications for how ABA companies recruit, message, and build career pathways for their direct care staff.
Several large providers have already built internal career ladder programs that treat the RBT role as the first rung of a clinical career. Hopebridge’s fellowship program enables graduate students to become RBTs while studying for the BCBA competency exams, and the company reports that clinicians who come through the fellowship have better retention and better clinical outcomes. ABA Centers of America funded 20 full-ride BCBA master’s scholarships through Temple University in 2024, with plans for 60 more in 2025. These programs recognize that the RBT role is most sustainable when it is positioned as a career step rather than a dead-end job.
The new BACB standards reinforce this trajectory. An RBT who is completing 12 CEUs per cycle, maintaining competency assessments, and investing in professional development is not a temporary worker—they are a developing clinician. Providers that reframe the role accordingly, with compensation, benefits, and career pathways that match the increased professional expectations, are likely to retain staff at higher rates. Providers that treat the new standards as a compliance burden without adjusting the employment value proposition are likely to see turnover accelerate.
The ABA industry enters 2026 at a crossroads on the RBT workforce question. The BACB has raised the bar. The clinical case for doing so is strong—better-trained, better-supervised, continuously-developing technicians will deliver better care. But the operational case depends entirely on whether providers absorb the cost as an investment in workforce quality or pass it through as an unfunded mandate that shrinks the candidate pool and accelerates attrition. For practice owners, clinical directors, and the PE sponsors backing them, the answer to that question will be one of the most consequential operational decisions of the year.
AT A GLANCE
| Effective date: | January 1, 2026 |
| New training: | 40-hour curriculum based on third edition Test Content Outline (BACB) |
| Renewal cycle: | Changed from annual to biennial (every two years) |
| Professional development: | 12 PDUs/CEUs required per two-year renewal cycle |
| Application fee: | Increased from $50 to $65 |
| Renewal fee: | $50 per two-year cycle (previously $35 annually) |
| RBT certificants (Oct 2025): | 232,792 (BACB) |
| Industry median turnover: | 65% for direct care staff (BHCOE, 2022 report) |
| CentralReach turnover data: | 76.7%–90.1% field-wide (2025–2026 Market Report) |
| BACB exit survey (2025): | 44% reported poor treatment; 27% felt isolated |
| Children with ASD per RBT: | Approximately 9.6 (rough ratio; ATCC/BACB data) |
SOURCES & REFERENCES
| 1. | Behavioral Health Business. “New RBT Standards Bring Operational Hurdles and Reimbursement Opportunities.” January 5, 2026. bhbusiness.com. |
| 2. | BACB. “Upcoming Changes.” bacb.com/upcoming-changes. Accessed March 2026. |
| 3. | BACB. “RBT 2026 Requirements.” bacb.com. PDF. July 2025. |
| 4. | BACB. “RBT Professional Development/In-Service Training.” bacb.com. PDF. July 2025. |
| 5. | CentralReach. “RBT Certification: What’s Changing in 2026.” centralreach.com. Accessed March 2026. |
| 6. | ABA Training and Certification Center. “RBT in 2026: Salary, Demand, and BACB Training Requirements.” atcconline.com. January 2026. |
| 7. | BHCOE Accreditation. “2022 ABA Compensation & Turnover Report.” (Median tenure: 1 year; 65% turnover for direct care, 2021.) |
| 8. | CentralReach. “Autism and IDD Care Market Report: 2025 Recap & 2026 Outlook.” (Turnover: 76.7%–90.1%.) |
| 9. | ABA Resource Center. “Building a Stronger RBT Workforce: Insights from the BACB Exit Survey.” December 2025. abaresourcecenter.com. |
| 10. | Behavioral Health Business. “Autism Providers Forecast ‘More Stability in the Workforce’ in 2025.” February 2025. bhbusiness.com. |
| 11. | BACB. “BACB Certificant Data.” bacb.com. (232,792 RBT certificants as of October 2025.) |