A Problem That Keeps Families Up at Night
ACROSS THE UNITED STATES – the question comes up in nearly every intake. A parent describes a child who cannot fall asleep without extended caregiver presence, wakes multiple times through the night, rises before 5 a.m., or has never maintained a consistent sleep schedule. The clinical team nods. It is a familiar pattern. What is less consistent is what happens next — whether the ABA provider treats the sleep problem directly, refers it out, or documents it and moves on.
The prevalence of sleep disturbances in autistic children is one of the most replicated findings in the autism research literature. A 2019 meta-analysis published in the Journal of Autism and Developmental Disorders, drawing on data from multiple studies, found that between 50 and 80 percent of autistic children experience clinically significant sleep problems, compared to 9 to 50 percent in typically developing children. The most common presentations are difficulty falling asleep (sleep onset insomnia), frequent night waking, early morning waking, and irregular sleep-wake schedules. Co-occurring intellectual disability and sensory processing differences are associated with higher rates and greater severity.
The downstream effects of pediatric sleep disturbance are well-documented and extend beyond the child. Research published in the Journal of Child Psychology and Psychiatry and other peer-reviewed outlets has linked chronic sleep insufficiency in autistic children to increased behavioral challenges during waking hours, reduced learning and memory consolidation, heightened anxiety, and greater caregiver stress and parental sleep disruption. For ABA providers, this creates an important clinical observation: a child whose sleep is severely disrupted is a child whose treatment outcomes are likely to be compromised regardless of the quality of the daytime intervention. Sleep is not a separate problem from the treatment plan — it is a moderating variable for virtually everything else in it.
A child whose sleep is severely disrupted is a child whose treatment outcomes are likely compromised — regardless of the quality of daytime intervention. Sleep is not separate from the treatment plan. It is a moderating variable for everything in it.
Why Behavioral Interventions Lead the Evidence Base
Pediatric sleep treatment broadly divides into two categories: pharmacological and behavioral. Melatonin is the most commonly used pharmacological intervention in autistic children, and a meaningful body of evidence, including a 2021 randomized controlled trial published in the Journal of Child Psychology and Psychiatry, supports its efficacy for sleep onset latency in this population. However, melatonin addresses sleep initiation but does not restructure the behavioral and environmental conditions that sustain broader sleep dysregulation. It is also not effective for all sleep problem subtypes, and prescribing authority rests with physicians, not BCBAs.
Behavioral sleep interventions have a stronger and broader evidence base for pediatric populations generally, and a growing evidence base specifically in autism. The core protocols — graduated extinction (sometimes called the Ferber method in popular usage), extinction with parental presence, faded bedtime with response cost, sleep restriction, and stimulus control therapy — target the behavioral and environmental variables that maintain sleep problems: conditioned parental presence, reinforcement of night waking, inconsistent sleep schedules, and maladaptive sleep-onset associations.
The BCBA scope overlap is direct: graduated extinction is a differential reinforcement and extinction protocol applied to a specific behavioral topography. Faded bedtime uses shaping. Stimulus control therapy restructures the discriminative stimuli associated with the sleep environment. These are not novel or specialized techniques requiring additional licensure — they are core ABA methodology applied in a new context. A BCBA competent in behavior analytic principles has the technical foundation to implement them; the question is whether they have the domain-specific knowledge of sleep science and the assessment tools to do so accurately.
A 2020 systematic review published in Sleep Medicine Reviews by Malow and colleagues examined behavioral sleep interventions in autistic children and found consistent evidence of efficacy across multiple protocols, with parent-mediated interventions showing particular promise for reducing parental burden while maintaining treatment effects. Research by Vriend and colleagues, published in the Journal of Pediatric Psychology, similarly documented improvements not only in sleep outcomes but in daytime behavior ratings following behavioral sleep intervention — a finding with direct relevance to ABA treatment teams monitoring behavioral targets.
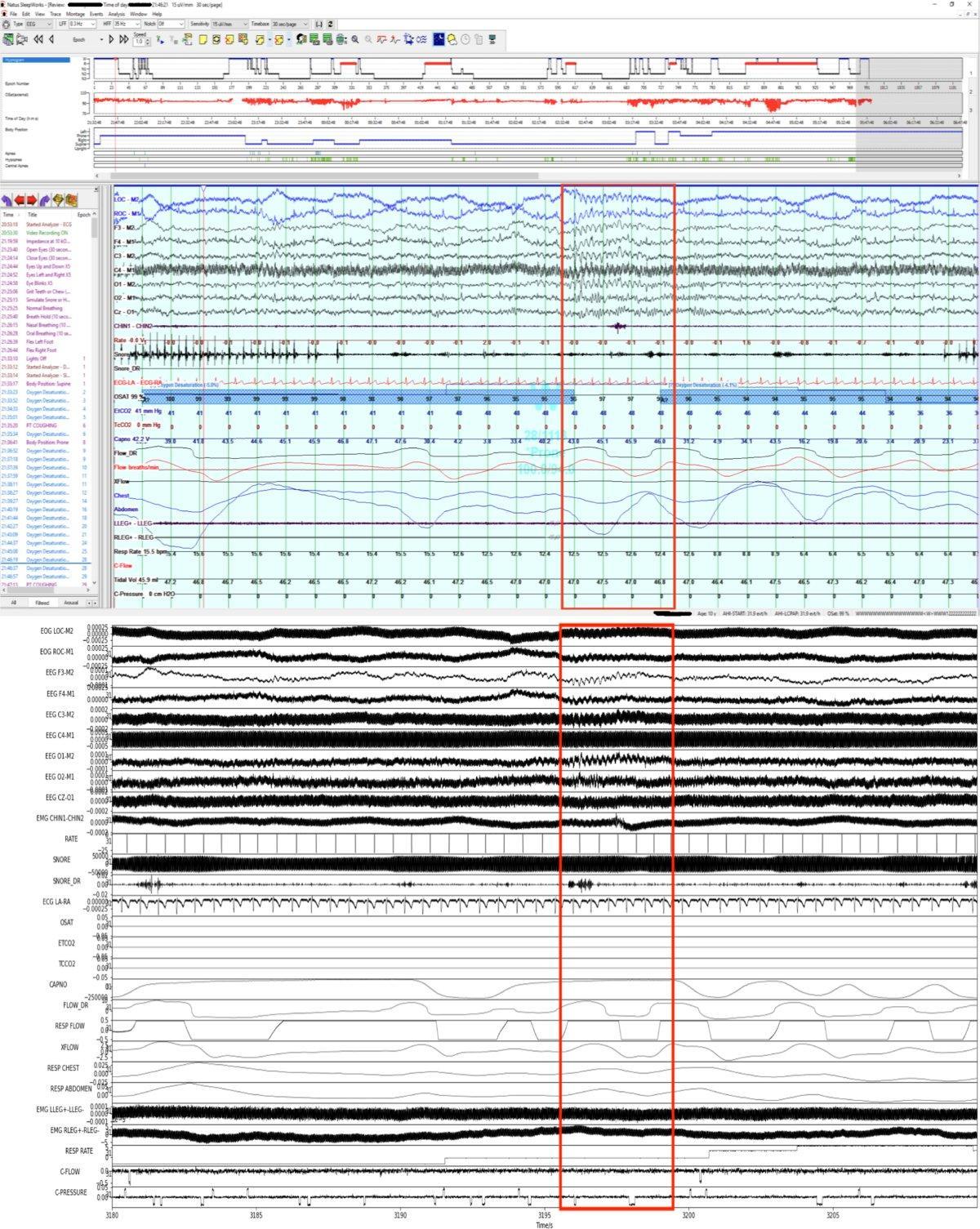
The Assessment Gap: What BCBAs Need That Training Often Omits
The theoretical alignment between behavioral sleep intervention and ABA methodology is clear. The training gap is equally clear. Standard BCBA preparation, as defined by the BACB’s Fifth Edition Task List, does not include sleep science, circadian biology, or the administration of validated sleep assessment instruments. A BCBA entering clinical practice has generally received no formal training in distinguishing behaviorally maintained sleep problems from those with an underlying physiological or medical etiology — a distinction that is clinically critical.
Sleep-disordered breathing, including obstructive sleep apnea, is prevalent in autistic children at elevated rates compared to the general pediatric population. Research published in Pediatrics has documented associations between autism and obstructive sleep apnea, and untreated sleep apnea produces behavioral presentations — hyperactivity, inattention, irritability — that overlap substantially with ASD symptom profiles. A BCBA who initiates a behavioral sleep intervention without ruling out obstructive sleep apnea is treating the behavioral surface of a medical condition, which may delay appropriate medical referral and exposes the provider to professional and liability risk.
The practical implication is that competent BCBA involvement in sleep treatment requires a collaborative medical screening step that the BCBA cannot perform independently. In well-functioning care teams, this means a standing protocol for requesting pediatrician or sleep medicine review before initiating behavioral sleep intervention. In the more common scenario where the ABA provider is operating with limited physician coordination, it requires the BCBA to explicitly scope their assessment, document what has and has not been ruled out, and make referral recommendations part of the written treatment plan.
Assessment tools in use: The Children’s Sleep Habits Questionnaire (CSHQ), developed by Owens and colleagues and published in Sleep in 2000, is a validated parent-report instrument with established cut-scores for clinical concern in school-age children. The Brief Infant Sleep Questionnaire (BISQ) and the Pediatric Sleep Questionnaire (PSQ) address different age ranges and clinical questions. Sleep diaries — nightly caregiver logs of bedtime, sleep onset, night wakings, and rise time — provide the behavioral baseline data most directly analogous to the data collection systems BCBAs already use. Actigraphy (wrist-worn movement monitoring) provides more objective data but requires equipment and interpretation expertise that most ABA practices do not currently have in-house.
Competent BCBA involvement in sleep treatment requires a collaborative medical screening step that the BCBA cannot perform independently. The liability risk of treating behavioral surface features without ruling out medical etiology is real.
How Practices Are Building Sleep Into the Service Model
A subset of ABA providers has moved beyond ad hoc sleep consultation and built structured sleep intervention into their clinical service model. The approaches vary by practice size, clinical team composition, and payer context, but several models have emerged as practical frameworks.
The most common model is caregiver-mediated behavioral sleep intervention delivered through parent training. The BCBA conducts a sleep-specific assessment, develops a written behavioral sleep plan, and delivers the intervention through caregiver coaching rather than direct therapist-to-child sessions. This model is consistent with how parent-mediated behavioral interventions are structured throughout ABA practice, and the evidence base specifically supports parent-mediated sleep intervention as effective. It also maps to existing CPT billing codes for parent training, though documentation requirements and payer-specific coverage policies for sleep-focused parent training vary and should be verified individually.
Larger practices and those affiliated with multidisciplinary clinical teams have developed more formalized sleep programs, sometimes in partnership with pediatric sleep medicine programs or developmental pediatrics practices. These arrangements allow the BCBA to manage the behavioral intervention while a physician or nurse practitioner manages medical screening and, where indicated, pharmacological adjuncts. The clinical logic is sound; the business case depends on whether the referral relationships can be formalized in ways that support patient flow without introducing insurance authorization complexity.
Training is the rate-limiting variable for most practices. BCBAs who want to competently deliver behavioral sleep intervention need domain-specific continuing education — not just in the behavioral protocols but in sleep science fundamentals, common pediatric sleep disorders, and the boundaries of their own competence. The BACB’s 2022 Ethics Code, Section 1.05, requires behavior analysts to practice only within their areas of competence, and to take steps to acquire competence through training and supervision before expanding into new clinical domains. Sleep intervention is precisely the kind of expansion that requires deliberate preparation rather than assumption that behavioral expertise transfers automatically.
For practice owners evaluating whether to formalize sleep services, the business case rests on three factors: the prevalence of sleep problems in the existing caseload, the degree to which unaddressed sleep disruption is limiting treatment progress on other targets, and the competitive differentiation value of offering a service that most ABA providers currently do not. The clinical case requires no such evaluation — the evidence that sleep quality moderates ABA treatment outcomes is robust enough that treating sleep problems as outside the scope of ABA practice is increasingly difficult to justify on clinical grounds.
AT A GLANCE
Sleep problem prevalence in autism: 50–80% of autistic children, vs. 9–50% in typically developing children (JADD meta-analysis, 2019)
Most common presentations: Sleep onset insomnia, night waking, early morning waking, irregular sleep-wake schedules
Daytime behavior link: Chronic sleep disruption associated with increased behavioral challenges, reduced learning, elevated caregiver stress (JCPP, multiple studies)
First-line pharmacological option: Melatonin — evidence supports efficacy for sleep onset latency; prescribing authority requires physician
Core behavioral protocols: Graduated extinction, faded bedtime with response cost, stimulus control therapy, sleep restriction, extinction with parental presence
BCBA scope alignment: Core protocols are extinction, shaping, and stimulus control applied to sleep context — within standard behavior-analytic methodology
Medical screening requirement: Obstructive sleep apnea must be ruled out before initiating behavioral sleep intervention; BCBA cannot perform this independently
Key validated assessment tool: Children’s Sleep Habits Questionnaire (CSHQ); Owens et al., Sleep, 2000 — validated for school-age children with clinical cut-scores
Parent-mediated model evidence: Malow et al. (2020, Sleep Medicine Reviews) found parent-mediated behavioral sleep intervention effective with durable effects
Daytime behavior improvement: Vriend et al. (Journal of Pediatric Psychology) documented improved daytime behavioral ratings following behavioral sleep intervention
BACB ethics requirement: Ethics Code Section 1.05 requires documented competence before expanding into new clinical domains including sleep intervention
Billing pathway: Parent training CPT codes most applicable; payer-specific coverage for sleep-focused parent training requires individual verification
SOURCES & REFERENCES
1. – Mannion A, Leader G. “Sleep Problems in Autism Spectrum Disorder: A Literature Review.” Review Journal of Autism and Developmental Disorders. 2014;1(2):101–109. doi:10.1007/s40489-013-0009-y
2. – Reynolds AM, Malow BA. “Sleep and Autism Spectrum Disorders.” Pediatric Clinics of North America. 2011;58(3):685–698. doi:10.1016/j.pcl.2011.03.009
3. – Cortesi F, Giannotti F, Ivanenko A, Johnson K. “Sleep in Children with Autistic Spectrum Disorder.” Sleep Medicine. 2010;11(7):659–664. doi:10.1016/j.sleep.2010.01.010
4. – Gringras P, Nir T, Breddy J, Frydman-Marom A, Findling RL. “Efficacy and Safety of Pediatric Prolonged-Release Melatonin for Insomnia in Children with Autism Spectrum Disorder.” Journal of the American Academy of Child & Adolescent Psychiatry. 2017;56(11):948–957.e4. doi:10.1016/j.jaac.2017.09.414
5. – Malow BA, Findling RL, Schroder CM, et al. “Sleep, Growth, and Puberty After 2 Years of Prolonged-Release Melatonin in Children with Autism Spectrum Disorder.” Journal of Child Psychology and Psychiatry. 2021;62(5):590–600. doi:10.1111/jcpp.13334
6. – Malow BA, Adkins KW, Reynolds A, et al. “Parent-Based Sleep Education for Children with Autism Spectrum Disorders.” Journal of Autism and Developmental Disorders. 2014;44(1):216–228. doi:10.1007/s10803-013-1866-z
7. – Malow B, Findling RL, Schroder CM, et al. “Behavioral Treatments for Sleep Problems in Children with ASD.” Sleep Medicine Reviews. 2020;53:101330.
8. – Vriend JL, Corkum PV, Moon EC, Smith IM. “Behavioral Interventions for Sleep Problems in Children with Autism Spectrum Disorders: Current Findings and Future Directions.” Journal of Pediatric Psychology. 2011;36(9):1017–1029. doi:10.1093/jpepsy/jsr044
9. – Owens JA, Spirito A, McGuinn M. “The Children’s Sleep Habits Questionnaire (CSHQ): Psychometric Properties of a Survey Instrument for School-Aged Children.” Sleep. 2000;23(8):1043–1051.
10. – Behavior Analyst Certification Board. Ethics Code for Behavior Analysts. Section 1.05: Practicing Within Competence. Effective January 1, 2022. bacb.com/ethics-codes
11. – Behavior Analyst Certification Board. BCBA/BCaBA Task List, Fifth Edition. 2017. bacb.com
12. – Bruni O, Alonso-Alvarez ML, Besedovsky L, et al. “Current Role of Melatonin in Pediatric Neurology: Clinical Recommendations.” European Journal of Paediatric Neurology. 2015;19(2):122–133. doi:10.1016/j.ejpn.2014.12.007